Care of Casts and Splints

Cast Care Do’s and Don’ts
Keep it dry
Care of Casts and Splints – If you haven’t been told specifically that your cast is waterproof it’s essential to keep it dry. Also note that even if your cast is waterproof that isn’t a license to get it soaking wet. You should still make every effort to keep water from getting between the cast and your skin. This is a sure recipe for an uncomfortable and sometimes smelly situation. Remember that you’re going to be wearing your cast for some time, so comfort is important.
Limit walking
Even with newer, non-plaster cast materials, your cast won’t fully harden for 2-3 days. It’s important to avoid weight bearing during this time, provided that you should be bearing weight at all. This is especially true on hard surfaces. If your cast becomes dented, it can cause pressure sores to form. Be careful and use common sense. In general, not bearing weight on the injured limb for 48 hours is recommended. This holds true even if you’ve been given a walking cast.
Elevate when possible
When you’re resting, try to keep the casted limb elevated above heart-level. This helps counteract the pull of gravity, and is especially important if you’ve got a leg cast. This will limit swelling and make sure your cast isn’t uncomfortably tight. Again, you’re going to be wearing your cast for some time, so comfort is paramount.
Take it easy
When casted, use the opportunity to take it easy. Don’t put too many demands on your injured limb, and certainly don’t do anything which could re-injure it. It’s your cast’s job to protect your limb, but it does require your cooperation.
Care of Casts and Splints -What to watch out for when wearing a cast:
Cast are a simple, safe, and effective method of immobilizing an injured limb, allowing it time to heal. Your time wearing one should be uneventful, but contact your doctor if you observe any of the following:
Any new pain.
If you’ve got a cast, then your injury itself is probably somewhat painful. If the pain gets steadily worse, however, it’s probably a sign that your cast is too tight. This can become quite painful, and is relieved somewhat relieved by elevation. If this is the case, simply contact your doctor’s office for a change of cast.
Bluish toenails or fingernails.
Beneath your nails lies what is known as the nail bed, which is usually pink due to good circulation. To test this, press down on one of your healthy nails. The nail bed should turn white as blood is forced from it, yet should turn pink again within seconds. This is known as the blanching response.
If the nails on your casted limb fail this test, or are gaining a bluish tint, contact your doctor immediately. This probably indicates that your cast is too tight and that you should be re-casted. An impaired blanching response is still a sign of reduced circulation, so be sure to bring this to your doctor’s attention even if this is the only symptom you’re having.
Numbn
If local anesthetics were used when your bone was set, some numbness in the following hours is normal. If this continues or becomes worse, however, contact your doctor. As with an impaired blanching response, numbness and tingling probably means that your cast is too tight. In rare cases this can also be a sign of nerve damage. As with an impaired blanching response, it’s important to run this past your doctor to rule out something more ominous.
Finger or toe movement restriction.
It’s normal to have some difficulty moving your fingers or toes due to your injury. If you’ve lost the ability to move them entirely, however, consult your doctor immediately. This is probably another symptom of an overly tight cast, yet in very rare cases it can signal nerve damage.
Fingers or toes which are cool to the touch.
It’s normal for patients to notice a slight temperature difference in the digits of the casted limb. This is usually due to the simple fact that you’re not using the limb as much as normal. As with the above situations, it’s probably a sign that your cast is too tight, but this is still a sign of impaired circulation. It’s best to err on the side of caution and call your doctor’s office.
Excessive Swelling
Keep your limb elevated above heart level is a good way to limit swelling. In fact, it’s normal for most injuries to cause some degree of temporary swelling. Make sure to tell your doctor if swelling persists or increases though. This can potentially be a sign that your cast is too tight. You’ll still want your doctor to rule out any other problems though, however unlikely.
Visibly damaged cast.
If your cast shows outward signs of damage have it checked out immediately, even if it’s close to your next checkup. Even small cracks can mean that your cast is weakened and isn’t performing its task of protecting your injury. In cases such as this, it’s best to be overly cautious and have the cast replaced.
What To Avoid?
When you have a cast or splint, it is important to take proper care of it to ensure proper healing of the injured area. Here are some things to avoid:
Getting the cast or splint wet: Moisture can weaken the cast or cause skin irritation, so it’s important to keep it dry. Avoid swimming, taking baths, or showering without covering the cast or splint with a waterproof cover.
Applying pressure: Do not put pressure on the cast or splint as this can cause it to shift or become loose. Avoid resting heavy objects on it or using it as a tool to lift heavy items.
Scratching or poking: Itching can be common underneath the cast or splint, but avoid scratching or poking it with sharp objects as this can cause injury or infection.
Removing it without medical supervision: Never attempt to remove the cast or splint yourself as this can cause further damage to the injured area. Always seek medical advice on when and how to remove it properly.
Modifying it: Do not alter the cast or splint in any way as this can also cause complications in the healing process. Avoid cutting, trimming, or bending it.
Not exercising: While it’s important to avoid putting stress on the injured area, it’s also important to continue to exercise other parts of your body to prevent muscle atrophy and maintain your overall physical health. Consult with your doctor or physical therapist for safe exercise options.
Ignoring signs of discomfort: If you experience persistent pain, swelling, or other signs of discomfort, it’s important to seek medical attention immediately as this may indicate a problem with the healing process or an underlying condition.
Taking proper care of your cast or splint involves avoiding moisture, pressure, scratching or poking, improper removal, modification, lack of exercise, and ignoring signs of discomfort. By following these guidelines, you can ensure proper healing and a speedy recovery.
Pins and Needles Feeling inside a Cast
Care of Casts and Splints
Fiberglass Cast Application
Types of Casts: Fiberglass vs Plaster Casts
Types of Splints and Casts
Casts are custom-made. They must fit the shape of your injured limb correctly to provide the best support. Casts can be made of plaster or fiberglass — a plastic that can be shaped.
Splints or half-casts can also be custom-made, especially if an exact fit is necessary. Other times, a ready-made splint will be used. These off-the-shelf splints are made in a variety of shapes and sizes, and are much easier and faster to use. They have Velcro straps which make the splints easy to put on, take off, and adjust.
 Materials
Materials
Fiberglass or plaster materials form the hard supportive layer in splints and casts.
Fiberglass is lighter in weight and stronger than plaster. In addition, x-rays can “see through” fiberglass better than through plaster. This is important because your doctor will probably schedule additional x-rays after your splint or cast has been applied. X-rays can show whether the bones are healing well or have moved out of place.
Plaster is less expensive than fiberglass and shapes better than fiberglass for some uses.
Care of Casts and Splints -Application
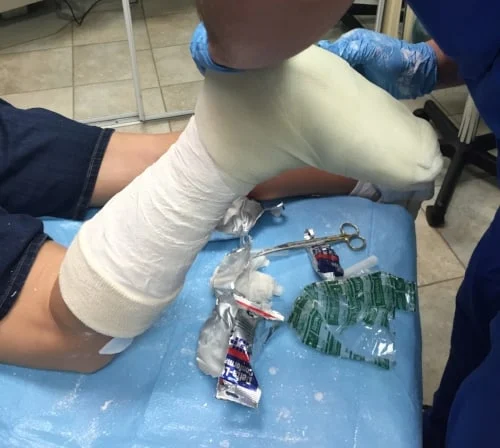
Both fiberglass and plaster splints and casts use padding, usually cotton, as a protective layer next to the skin. Both materials come in strips or rolls which are dipped in water and applied over the padding covering the injured area.
The splint or cast must fit the shape of the injured arm or leg correctly to provide the best possible support. Generally, the splint or cast also covers the joint above and below the broken bone.
Apply a splint to a fresh injury first. As swelling subsides, a full cast may replace the splint.
Replace a cast as swelling goes down and the cast gets “too big.” As a fracture heals, replace the cast with a splint to make it easier to perform physical therapy exercises.

 Materials
Materials