Athlete’s Foot Treatments

Athlete’s Foot Treatments – Serving the Greater Pittsburgh Area
FOOT FUNGUS DISEASE PITTSBURGH
Athletes Foot Causes and Treatments Cranberry Twp
Athlete’s Foot treatments for one of the most common conditions on the skin of the foot that a Podiatrist in Beaver sees every day. From Teenage athletes to runners to our aged veterans athletes foot is umbiquitous!
Athletes foot is a fungal infection of the skin of the foot.
It is EVERYWHERE! And it loves the warm dark moist sneakers that wear all day.
 Podiatrist in Moon Twp who treats Athletes Foot
Podiatrist in Moon Twp who treats Athletes Foot
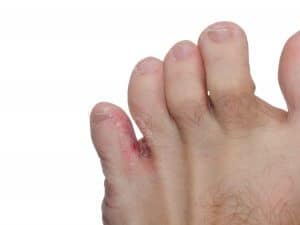
Athlete’s foot between toes
There are two common types of foot fungal infections. The first is acute athletes foot and chronic athletes foot is the second. Acute athletes foot has red little pimples or blisters. They are red, itchy or burning. You find this between toes, on the bottom and sides of the feet and can even creep up your legs. In older athletes, or vets who suffered trench foot in the war, the condition is often chronic. This appears as dry scaly feet, sometimes white and scaling. Often patients mistake chronic athletes foot as dry feet and can cause very painful cracked heels.
Athlete’s Foot Treatments (tinea pedis)
Athlete’s foot is an extremely common fungal infection of the feet and toes. The fungus which causes it thrives in warm, moist conditions such as locker rooms and showers. Hence the name “athlete’s foot.” Podiatrist Pittsburgh treat athletes foot more effectively than most family doctors.
Basic Athlete’s Foot Treatments Information
Q: What exactly is athlete’s foot?
Answer: Athletes foot is one of the most common fungal infections of the foot podiatrist near me treat. It’s highly infectious, meaning you can both catch it and spread it to others. The fungus responsible for causing this infection does well in warm, moist environments. Examples include locker rooms, showers, and inside sweaty athletic shoes.
- The medical name for athlete’s foot is tinea pedis.
- Symptoms of infection include dry, cracked, irritated skin, especially between the toes. Redness is visible in most cases.
- About 20% of people will have at least one case of athlete’s foot in their lives.
- Foot fungus is relatively easy to cure by a Foot Doctor near me with our Athlete’s Foot Treatments. Topical antifungal medicine such as powders and creams readily cure athletes foot.
- Although we know it popularly as athlete’s foot, it infects plenty of non-athletes as well.
- Many people with athletes foot also get fungus toenails.
As mentioned, we manage athletes foot usually with over the counter antifungal preparations. If these aren’t sufficient however, Lamisil is effective in almost 100% of tinea pedis cases, which is prescribe by a Podiatrist near me.
Q: After I finish my treatment is it possible for the fungus to infect the skin again?
A. It’s possible, but you can lower your chances by practicing good foot hygiene (see below). Lamisil also provides a window of protection for up to 3 months after you’ve finished treatment.

Q: How common is athlete’s foot?
A: Athletes foot, or tinea pedis, is extremely common. Tinea will affect 20% of Americans at some point during their lives. Repeat infections are possible and can occur frequently in some people. Your local Podiatrist is the best doctor to treat athlete’s foot.
Q: What Are Athlete’s Foot Symptoms ?
A: There are so many symptoms of athlete’s foot so if think you are suffering from it you should look for these symptoms:
• Discolored, crumbly or thick nails
• Blisters
• Discoloration of the skin
• Experiencing itching and burning between your toes
• Cracks in between your toes
• Peeling of the skin
• Loose toenails that can be pulled away from the nail bed
• Dry skin
If you notice any of the above symptoms its best to get medical treatment as soon as possible or the symptoms might get worse.
Q: What Are Risk Factors Of Athlete’s Foot?
A: Some situations can make this problem more likely to affect you, these situations and called risk factors, here are some risk factors of athlete’s foot:
• Sweating often, especially from feet
• Walking without shoes or slippers in areas like swimming pools and gyms, since these areas contain a lot of germs and infection causing bacteria.
• Receiving nail clippers, clothes and mats from a person infected with athlete’s foot.
• Wearing shoes that don’t provide enough space.
• Skin or nail injuries
• Toenail disorders like nail fungus.
Q: Is Athlete’s Foot Preventable?
A: Yes, you can prevent athlete’s foot easily since all you need to do is follow these tips:
• Avoid sharing nail clippers, socks, shoes and clothes with others
• Always wear shoes, slippers or sandals around places like public showers, swimming pools and gyms.
• Wash your feet everyday with soap and dry them properly and don’t forget to prevent moisture between your toes.
• Wear shoes that provide a lot of space and do same with socks as well.
• Change your socks and wash them, if they get sweaty and if that’s not possible then then wear moisture wicking socks.
• If you have any problems like nail fungus then treat them as soon as possible!
• Listen to your doctor and take all your medicines.
Q: How easy (or difficult) is it to become infected?
If I come into contact with the fungus will I get athlete’s foot 100% of the time?
Exposure doesn’t necessarily mean infection will occur. If you believe you have exposure, however, you should practice good foot hygiene if you aren’t already doing so. It’s often a good idea to start using over the counter fungicide powder or cream as a preventative measure.
Q: Is proper hygiene the best way to prevent athlete’s foot?
A. Absolutely. Follow these tips to greatly reduce your chances of infection:
· Both wash and dry each foot thoroughly, especially between the toes.
· Don’t wear the same shoes on a daily basis for an extended period of time. This allows your shoes to dry completely.
If you naturally sweat a lot or are very active it’s a good idea to change socks at least once daily. Use a powder, cream, or spray antifungal daily to prevent infection. Never walk barefoot in locker rooms, showers, or around pools or hot tubs. Always wear sandals or surf shoes.

Q. Will athlete’s foot go away on its own?
A. In the majority of cases it won’t go away. Good foot hygiene is always important. If fungus infects your skin already, then it’s not a cure. Athlete’s Foot Treatments like topical antifungal medication, either over the counter or prescriptions like Lamisil, are usually required.
Q. Is there a best time to apply topical antifungal medication?
A. It’s best to use these athlete’s foot treatments medications both in the morning and at night before bed. Always make sure your feet are clean and dry before applying.
cracked heel cream 20% Urea Cream for Dry Feet, Moon Twp
Similar Fungal Organisms Infect the Skin as Well as the Nails

Many patients with athletes foot, if left untreated for an extended period of time eventually end up with the organism invading the nail. Several types of fungal organisms can infect fingernails and toenails. This most often happens to the nail of the great toe, yet can occur on the other toes or even on fingernails. The commonly known infection is toenail fungus. We technically know it as onychomycosis.
Dermatophytes are by far the type of fungus responsible for most infections, although some types of yeasts and molds cause them as well.
The skin’s dead outer layers initially confined this type of fungus. Eventually it can more or less take over the entire nail. Once the infection reaches the living nail bed beneath the hard outer nail, the condition is severe and the nail may be in danger. Anyone can get fungal nails. They’re most common in older men for a variety of reasons. Fungus is difficult to treat since the nail actually protects the fungus under the nail plate. Any medication we use will have problems reaching the actual infection.
How is Fungus Treated?
Since this type of infection is generally confined to the superficial (shallow) layers of the skin, it would seem that they’re easy to treat. That topical creams and ointments should work well. In fact this isn’t true at all. As mentioned, the nail protects the underlying fungus, just like it protects the sensitive underlying skin–it’s a relatively sealed, impervious barrier.
Here’s another consideration. In many cases, toenail fungus doesn’t produce any symptoms other than an unsightly appearance. Therefore, in most cases, the only real criteria in determining whether or not to treat is how much these cosmetic concerns bother a patient. Because of this, here’s what a perfect toenail fungus treatment would look like–it’d be inexpensive, safe, entirely effective and with no side effects, and work quickly. Needless to say, medical science has yet to achieve this.
Will laser therapy for my toenail fungus really work?
Technically known as onychomycosis, toenail fungus is as common as it is stubborn. By some estimates about 10% of Americans have some level of infection, and many products advertise a “cure,” yet fall far from the mark. It’s because the fungus often lives under the nail.
The picture gets worse with age. Experts estimate that over half of all adults over 70 have an active infection. This is largely due to the simple fact that the older a person is, the longer they’ve been exposed to these infection causing fungi.
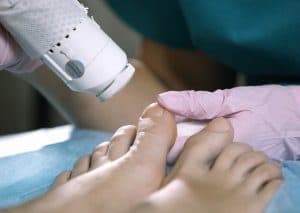
Side effects of Fungus Medicine?
Many studies have found that laser treatment is viable while having very minor to no side effects, especially compared to the oral medications available
Can I still exercise if I have athlete’s foot?
Yes, you can still exercise if you have athlete’s foot, but it’s important to take precautions to prevent spreading the infection. Here are some tips:
1. Keep Your Feet Dry: Moisture can worsen athlete’s foot, so be sure to dry your feet thoroughly after exercising and change into clean, dry socks and shoes.
2. Wear Proper Footwear: Choose breathable shoes and moisture-wicking socks to help keep your feet dry during exercise.
3. Use Antifungal Powder: Consider using an antifungal powder on your feet and in your shoes to help prevent the spread of the infection.
4. Avoid Barefoot Exercise: If possible, avoid exercising barefoot in public areas to reduce the risk of spreading athlete’s foot to others.
5. Wash Your Hands: Be sure to wash your hands thoroughly after touching your feet to prevent spreading the infection to other parts of your body or to others.
Can I get athlete’s foot from someone who has it?
Yes, athlete’s foot is contagious and can be spread from person to person. The fungus that causes athlete’s foot thrives in warm, moist environments such as locker rooms, showers, and swimming pools. You can contract athlete’s foot by coming into contact with surfaces or objects that have been contaminated with the fungus, or by direct contact with someone who has the infection.
Is It safe to treat athlete’s foot during pregnancy?
It is generally safe to treat athlete’s foot during pregnancy, but it’s important to consult with a healthcare professional before starting any treatment, especially if you are pregnant or breastfeeding. Some antifungal medications may not be recommended during pregnancy due to potential risks to the fetus. Your healthcare provider can recommend safe and effective treatments for athlete’s foot that are suitable for use during pregnancy.
Is There A Risk Of Allergic Reactions To Athlete’s Foot Treatments, And How Can I Minimize This Risk?
Yes, when treating athlete’s foot there’s a risk of allergic reactions however it’s really uncommon. The allergy can happen because of the ingredients and components in the medication, here are few steps to help you prevent the risk of allergies:
1. Read the labels carefully
Make sure you read the labels on the medication really carefully, if you notice any ingredients that can cause allergies then it wouldn’t be a good idea to take that medication.
2. Patch Test
Try applying a small amount of the treatment to a less sensitive area of the skin for at least 24 hours and see if you notice any redness, swelling or irritation. It can help you out if the treatment is safe for you or not.
3. Talk to your doctor
It’s always a good idea to be honest about your allergies to your doctor, especially since they will help you get the best treatment possible based on your situation.
4. Choose Hypoallergenic products
Look for products labeled as hypoallergenic, fragrance-free and designed for sensitive skin.
5. Monitor your symptoms
Be alert about any signs like skin irritation, itching, swelling or redness on the treated area, do not ignore it for too long if it happens. If these symptoms are notice, avoid the use of medications immediately.
6. Alternative Treatments
If your condition isn’t too severe then maybe you can fix it on your own by using home remedies like tea tree oil, apple cinder vinegar, or garlic. But be aware that these can also cause allergic reactions, so use them carefully and avoid using them if you notice any symptoms of discomfort.
7. Follow the instructions
Sometimes it’s not the component, but the usage. Overdose can also lead to allergic reactions to use them as advised.