Tendonitis Ankle

Tendonitis ankle (peroneal tendinosis):
 Tendonitis is the technical term for the chronic inflammation and irritation of a tendon anywhere in the body. When this occurs in the ankle it’s known simply as ankle tendonitis or more formally as peroneal tendinosis. Regardless of what it’s called, this condition involves either of two specific tendons which cross the ankle joint. This type of overuse injury is seen in all types of athletes yet is most common in long distance runners.
Tendonitis is the technical term for the chronic inflammation and irritation of a tendon anywhere in the body. When this occurs in the ankle it’s known simply as ankle tendonitis or more formally as peroneal tendinosis. Regardless of what it’s called, this condition involves either of two specific tendons which cross the ankle joint. This type of overuse injury is seen in all types of athletes yet is most common in long distance runners.
What causes tendinitis of the ankle?
Tendons are the thick, tough connective tissue bands which cross joints and connect muscles to nearby bones. When these muscles contract they exert a pulling force through the tendons which allows the joints to move. Along with the Achilles tendon, the peroneus longus and peroneus brevis tendons both move and stabilize the ankle joint.
The peroneal tendons run behind the rear bones of the ankle. Together, they connect the smaller leg bone (fibula) to the heel bone (calcaneus). This provides stability during walking and running.
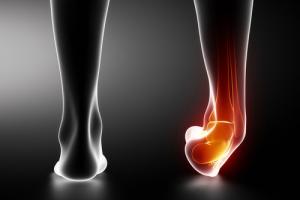
As mentioned, ankle tendonitis is an overuse injury resulting from what athletic trainers call “training errors.” These usually involve training too hard or not allowing enough rest between workouts. Another common training error is increasing workout intensity too quickly. Other risk factors include training without the proper footwear and running on sloped surfaces. Athletes who have weak calf muscles, high arches, or ankles which turn inward are particularly susceptible. In rare cases, peroneal tendinosis can be caused by a single acute injury such as a bad ankle sprain. Chronic inflammatory joint conditions such as arthritis can also contribute.
Signs and symptoms of ankle tendonitis:
In the vast majority of cases the symptoms of peroneal tendinosis start slowly and worsen over time. In its initial stages, an athlete may notice warmth, tenderness, and generalized swelling of the affected ankle. This typically progresses to mild-moderate pain at the posterior (rear) and lateral (side) aspects of the joint. These symptoms tend to increase with activity and temporarily improve with rest. Symptoms may appear worse in the morning and begin to lessen as the ankle joint “warms up.” Specific movements which exacerbate symptoms include pushing off on the ball of the foot and turning the ankle inward.
Preventing peroneal tendinosis:
Avoiding injuries is always preferable to treating them. This is especially true of overuse injuries which can take weeks or even months to heal. Doing so is mostly a matter of avoiding “training errors.”
- Maintain flexibility in your ankle, knee, and hip joints.
- Maintain strength and coordination in the muscles which move these joints.
- Always wear proper footwear when training or competing. Period. Change shoes as recommended—footwear may be expensive but avoiding injury is well worth the price.
- Don’t exercise beyond your level of conditioning. Train smart, and only increase the intensity or duration of your workouts when you’re ready.
- Don’t over-train. Make sure you’re getting enough recovery time between workouts.
- Get proper nutrition and drink plenty of water. This lets the micro-trauma that occurs with each workout heal quickly and completely.
- Only use braces or compression wraps when necessary. It’s an axiom among PTs and trainers that “braces help you become weak.
- Deal with injuries immediately after they occur. Seeking professional treatment instead of toughing it out is one of the smartest things any athlete can do.
 How is tendonitis of the ankle treated?
How is tendonitis of the ankle treated?
Left untreated, ankle tendonitis will almost always worsen with time. Furthermore, failing to treat the condition promptly increases the odds of a peroneal tendon tear. This is a much more serious injury. Early intervention leads to the best outcomes. It’s best to seek treatment as soon as symptom appear.
Diagnosing peroneal tendinosis (or any other sports injury) should only be done by a trained Pittsburgh podiatrist near me. She will take a brief medical history and perform a physical exam including orthopedic and muscle testing. Specialized imaging such as MRIs and CT scans are rarely needed.
Once the diagnosis is reached, your Podiatrist near me will devise a treatment plan. Fortunately, this condition responds well to conservative treatment. Surgery is rarely necessary. In many cases RICE (see below) and physical therapy are all that’s required. It’s important to recognize that this is an overuse injury. Prolonged periods of rest may be required. This can be especially frustrating for competitive athletes yet is often what’s necessary for complete healing to occur. Below are the basic components of a conservative treatment plan.
The RICE approach to ankle tendonitis:
- Rest. This rarely refers to complete rest, e.g. not using the joint whatsoever. Relative rest, such as working out at a reduced intensity is usually sufficient. Lower impact activities such as swimming or cycling are often used to maintain conditioning as the injury heals.
- Ice. Cryotherapy using a cold compress or ice pack is a simple and effective way to reduce inflammation. Ice the joint down several times throughout the day, especially after a workout. Never apply cold directly to the skin or for longer than 20 minutes at a time.
- Compression. Wrapping the joint using a compression bandage can help reduce swelling while providing the joint with added support.
- Elevation. Another tried and true method for reducing swelling and inflammation. Simply elevate the joint whenever resting, preferably above the level of the heart.
Physical therapy and rehabilitation exercises:
Depending on the injury’s severity your physical therapist may or may not prescribe a supportive brace or boot. The therapy program itself will consist of components designed to reduce symptoms and improve function. Preventing re-injury is equally important. Your individual program will likely include some or all of the following:
Passive therapies:
physical therapists often employ what are known as adjunctive therapies or procedures to treat soft tissue injuries. These modalities are quite versatile and can be used as needed to control symptoms, improve circulation, and enhance healing. Some of the most widely used today include heat, ice, ultrasound, and manual soft-tissue manipulation. Such treatments are passive (as opposed to active), meaning that they’re performed on the patient by the therapist.
Manual joint mobilization:
this refers to a diverse group of hands-on techniques in which the PT passively moves a patient’s joints. Such mobilizations are used to enhance a joint’s range of motion by breaking up adhesions and scar tissue. They also allow patients to regain a sense what’s happening inside the joint as it moves. This is known as proprioception and is a critical part of the rehab process.
Range of motion exercises:
are often referred to simply as ROMs. These gentle motions help patients to regain flexibility while improving proprioception (see above). ROMs are almost always included in the early stages of a rehab protocol.
Strengthening exercises after Tendonitis Ankle:
this is what first comes to mind when most patients think of physical therapy. They rely on elastic bands bands, hand weights, and body weight to provide resistance. The primary goal of strengthening exercises is to regain muscle strength and endurance. When prescribing strengthening exercises the only real limitation is the physical therapist’s imagination.
Functional or function-specific training:
these exercises are designed to reinforce the motions unique to a particular athletic activity. This type of training is essential for an athlete’s safe return to their chosen sport.
Education:
this blanket term includes advice on how to avoid re-injury. It’s also common for physical therapists to help patients develop a “ramp up” training regimen.
Can ankle tendonitis lead to other complications if left untreated?
Yes, ankle tendonitis can lead to other complications if left untreated or if it becomes chronic. Some of the potential complications include:
- Tendon Rupture: If the tendonitis is severe and left untreated, it may weaken the tendon, making it more susceptible to complete rupture. This can be a significant and painful injury that may require surgical repair.
- Chronic Pain: Untreated ankle tendonitis can lead to ongoing pain and discomfort in the affected area. Chronic pain can interfere with daily activities and reduce quality of life.
- Ankle Instability: Tendonitis can weaken the ankle, affecting its stability. This instability may increase the risk of sprains, falls, and other injuries.
- Limited Range of Motion: As the inflammation persists, it can lead to scar tissue formation, which may restrict the ankle’s range of motion.
- Compensation Injuries: To avoid using the painful ankle, individuals may unconsciously alter their gait or movement patterns, leading to overuse injuries in other areas of the body, such as the knees, hips, or lower back.
- Bursitis: Inflammation of the tendons can sometimes irritate nearby bursae, small fluid-filled sacs that cushion and reduce friction between tendons and bones. This can lead to bursitis, causing additional pain and swelling.
- Tendinosis: Chronic tendonitis that goes untreated can progress to tendinosis, a condition characterized by degeneration and weakening of the tendon fibers. Tendinosis is more challenging to treat than acute tendonitis.
- Infection: In rare cases, an untreated or poorly managed ankle tendonitis can become infected, leading to a more serious health issue.
- Muscle Atrophy: Prolonged inflammation and reduced use of the affected ankle due to untreated tendonitis can lead to muscle atrophy. Muscle wasting and weakness can further impair ankle function and delay recovery.
- Chronic Tendinopathy: If ankle tendonitis becomes a long-standing issue without appropriate treatment, it can develop into chronic tendinopathy, which involves ongoing pain, degeneration of the tendon, and difficulty in healing.
Surgical intervention: Tendonitis Ankle
It’s a general rule that surgery is only appropriate when all conservative measures have failed. With this being said, modern orthopedic surgery is rapidly becoming less invasive and often proves quite effective.
Surgery can be thought of as a physical solution to a physical or problem. It’s almost always indicated when the peroneal tendons are mostly or fully torn. Bone spurs which cause ongoing irritation by rubbing against a tendon also usually respond well to surgery.
A program of physical therapy following any surgical procedure is a vital part of the recovery process. According to many PTs and quite a few surgeons “a procedure is only as good its rehab.”
Achilles Tendon Pain:
Causes and Treatment Options for Tendonitis Ankle
Do you have questions about Achilles tendon pain? We’re here to help.
Named after the Greek hero of the Trojan War, the Achilles tendon is a strong band of tissue in the back of the heel. Also called the calcaneal tendon, it connects the calf muscles (gastrocnemius) to the heel bone (calcaneus).
The Achilles tendon stands out as the largest and strongest tendon in the body. Although very strong, tendons are not very flexible, which makes them prone to injury. The Achilles may be particularly susceptible to injury, because of the high tensions placed on it and its limited blood supply. Like other tendons, the Achilles is only capable of extending so far before it tears or becomes inflamed. Inflammation in the Achilles is called tendonitis. If an Achilles tendon becomes damaged, it can cause a variety of symptoms. Symptoms can range from slight irritation, aches and tenderness to stiffness and severe pain. These are especially true when the foot is bent downward.
Heel Discomfort-Tendonitis Ankle
If you are experiencing any pain or discomfort in your heel, it is important to become familiar with the varied medical conditions that can affect the Achilles tendon. Although the pain may feel similar, the cause, diagnosis, and treatment can vary. Because of their unique causes, some will require urgent attention and therapy.
Achilles tendonitis and Achilles tendonosis are the two most common causes of Achilles tendon pain. While these conditions may sound very similar, don’t be fooled. They are completely different conditions. One is chronic while the other more acute.
Achilles Tendonitis ankle
First we will cover Achilles tendonitis. Achilles tendonitis most commonly affects athletes (especially runners, or people who play sports that require lots of starting and stopping, such as tennis). It is characterized as an acute, inflammatory injury of the Achilles tendon. Most sufferers present with pain. It is most frequently described as a burning sensation that worsens when the tendon is used. Depending on the specifics of each individual case, the location of the pain may vary. For some patients, it will present towards the bottom of the calf muscle. Others report the pain along the length of the actual tendon. While others experience the burning sensation lower in their leg, down near the heel bone.
Accompanying the pain, sufferers may experience mild swelling. The area may also feel warm to the touch. It is not uncommon to have stiffness in both the heel and calf when you first wake up in the morning. The tightness should get better as you start to warm up and stretch your leg and ankle.
If you were wondering, “what is the largest human body tendon? “
Achilles would be the answer. Where is the Achilles tendon located? The insertional Achilles tendon heel location is behind the foot, at the back of the heel. The “calf” is made up of the Gastrocnemius muscle belly and the Soleus muscle. The muscles end toward the bottom of the leg in the back, and become tendons. These two muscles’ tendons combine to form the Achilles tendon. This inserts into the back of the calcaneal bone (heel bone). So if you ask,” where is it achilles heel location?’ The akele tendon is between the calf muscle and the heel bone.
What is achilles injury or Tendonitis Ankle?
Pain in the heel of my foot. Treatment is determined by the location and extent. The age of the injury also plays a role. The back of heel pain treatment can range from simple to complex. Treatments from heel pain treatment at home, like icing, heel pain treatment home remedies and heel pain treatment exercises; to more involved treatment for heel pain, like injections or orthotic heel inserts. Treatment for plantar fasciitis heel pain and achilles heel pain treatment is very similar. The basis for treatment for plantar fasciitis heel pain and achilles heel pain treatment starts with ways to reduce the inflammation, immobilize and rest the area, then promote healing. Here at Beaver Valley Foot Clinic, we attack heel pain treatment from many angles all at once.

 How is tendonitis of the ankle treated?
How is tendonitis of the ankle treated?