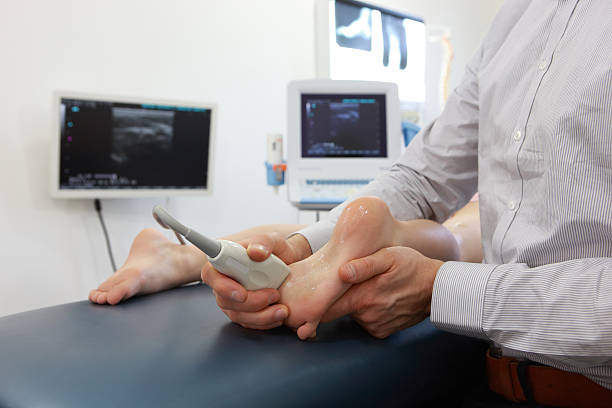
PRP Injection Therapy for Foot & Ankle Conditions

PRP Injection
Regenerative Medicine: Platelet Rich Plasma – PRP
– aids in complete healing of chronic foot and ankle injuries.
If you’ve never heard of regenerative medicine that’s understandable. This rapidly growing branch of specialty medicine has only become widespread within the last decade. Yet ironically several of the treatments used in regenerative medicine have been around for years.
Only recently, however, have advances in technology and technique rendered these treatments truly viable and effective. What’s more, only as our scientific understanding of the healing process grows have we been able to use these techniques to the most advantage. As such, regenerative medicine is an example of having a tool without the knowledge to unlock its full potential.
Common foot and ankle injuries treated with Platelet Rich Plasma (PRP) therapy.
Humans stand and walk upright, putting a tremendous amount of stress and strain on their ankles and feet feet. The reason is simple—we stand and walk upright, often for hours each day. This makes the joints, ligaments, and tendons in this area particularly vulnerable to overuse injuries.
Fortunately, this also makes them ideal candidates for PRP and other forms of regenerative medicine. These include:
- Arthritis—many cases of osteoarthritis, also known as “wear and tear” arthritis, respond well to PRP.
- Tendonitis and tendonosis—these common tendon injuries are often due to overuse, and PRP can help them heal properly.
- Sports injuries of the foot and ankles—PRP can stop the cycle of poor-quality healing and re-injury. The perfect example are ankles which sprain repeatedly, often spraining easier every time.
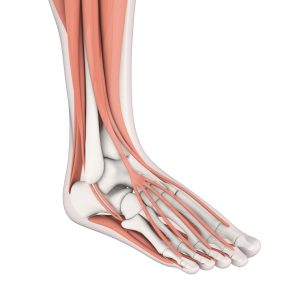
- Plantar fasciitis—the plantar fascia is the long, flat tendon located on the bottom of the foot. When it’s chronically inflamed it can’t heal properly, a chronic and often very painful condition known as plantar fasciitis. This condition is particularly notable because severe cases can interfere with walking, yet it responds very well to PRP.
- Muscle strains—muscles typically have a good blood supply and normally heal well. When this isn’t the case, especially when repeated injuries occur, PRP can often help.
- Ankle ligament injuries—many short, tough ligaments hold the bones of the foot and ankle together. When these are badly sprained or partially torn PRP can promote proper healing.
- Chronic foot and ankle pain—the pain associated with long-term foot and ankle injury can be significant. Once PRP is administered and the injured structures heal completely this pain can subside.
 Platelet Rich Therapy (PRP) Treatment for Chronic Tendon Injuries.
Platelet Rich Therapy (PRP) Treatment for Chronic Tendon Injuries.
Tendons are extremely resilient, cable like structures. They’re built for strength, and unfortunately this leather-like composition means they usually have poor circulation. This means that, once injured, tendons can heal slowly and in some cases not at all.
In recent decades, medical researchers have gained a greater understanding of cell biology and healing. This has translated into newer treatments which promote healing, even in structures without a good blood supply. Today, the most widely used of these regenerative medicine techniques is probably Platelet Rich Plasma (PRP) injections.
Both the technique and the specially prepared fluid used to perform it are usually known by the abbreviation “PRP.” Once this fluid has been prepared, it’s injected directly into an injured tendon. The stated goals of PRP include:
- Improving joint and limb function.
- Reducing the pain of chronic injuries
- Accelerating healing
- Improving the strength and quality of the newly regenerated tissue.
For a larger, more complicated injury it’s often necessary to use medical imaging techniques to guide treatment. This is especially true if the ligament is located beneath inches of tissue or adjacent to sensitive structures. In PRP treatments this usually refers to small veins, arteries, and nerve bundles. A good example of a larger, more complex injury which may require ultrasound guidance is a badly damaged rotator cuff.
Treatment with Platelet Rich Plasma concentrates is without traditional pharmaceutical side effects. It’s likely, however, that the treated area will be moderately sore in the days following the injections. Note that this is typical of any healing injury or wound, whether the healing is caused by PRP or not. This soreness typically lasts no longer than 4 days. If the treated joint is in the foot or ankle, meaning that it bears weight, your podiatrist will likely prescribe a supportive boot or brace. This provides stability and protection as delicate ligaments and tendons begin to heal.
Ironically, this research has shown that many formally diagnosed cases of tendinitis don’t involve much inflammation at all. Under an electron microscope it can be seen that this “inflamed” tissue has been structurally altered. Specifically, this refers to the breakdown of collagen fibers within the tendon. This makes the term “tendinosis” a much better fit.
As in any connective tissue, these collagen fibers naturally break down and are replaced at a fairly steady rate. If the tendon is chronically stressed, however, this can’t happen fast enough and damage begins to accumulate. This chronic damage isn’t inflammation, but it often causes ongoing pain and disability, both things associated with chronic inflammation. What’s more, it’s not uncommon for tendon injuries to have a structural component and an inflammatory component.
Confusing? Most certainly, but these distinctions are important. The underlying problem in many (if not most) tendon injuries is microscopic structural damage to collagen fibers, not inflammation. Today regenerative medicine techniques such as Platelet Rich Plasma (PRP) injections can be used to actively stimulate collagen production. Once the tendon is allowed to heal properly, physical symptoms such as pain, weakness, and instability begin to disappear.
PRP is a common sense solution to a structural problem. If inflammation were the cause, then steroids or Non-Steroidal Anti-Inflammatory Drugs like ibuprofen would be entirely effective. Instead, in the case of tendon or other soft-tissue damage like ligament sprains, PRP is usually a better and more permanent solution.
But what about tendinopathy?
Tendinopathy—note that “opathy” is the medical suffix referring to “disease or suffering.” As such, the term can technically be used to describe any tendon injury or disease of any type. In actual clinical practice, however, this term is rarely encountered.
So what term is typically used in its place? Tendinitis, of course.
Variability in patient tendon tissue:
Just as with blood, each patient’s tendons are somewhat or even substantially different. Furthermore, each tendon within an individual will be slightly different from surrounding tendons. This can also be said of each individual injury.
PRP – platelets
What’s more, PRP is created using a patient’s own blood platelets and therefore doesn’t rely on pharmaceutical drugs. Going further, the high-quality healing brought about by PRP injections can potentially allow patients to avoid surgery. This makes a combination of physical therapy and PRP a very good option for patients facing possible surgery.
Much as it sounds, the goal of regenerative medicine is to “make tissue heal,” or in other words regenerate. For obvious reasons this is preferable to most pharmaceutical drugs and (especially) surgery. To date, one of the mainstays of regenerative medicine is known as Platelet Rich Plasma injections, often abbreviated as “PRP.”
PRP is also notable because it doesn’t rely on artificial drugs or chemicals to stimulate healing. The Platelet Rich Plasma serums used are derived entirely from a patient’s own donated blood. As we examine the term itself—Platelet Rich Plasma—it will become apparent how this is done. It will also illustrate just exactly how efficient and ingenious the PRP approach truly is.
Platelets are extremely small particles found in abundance in human blood. These particles are unique because they aren’t living cells such as red, white, or amoeba-like macrophages. Platelets are many times smaller than these cell types, and serve the vital and indeed amazing function of allowing blood to clot. Without platelets and associated natural clotting factors even small cuts simply would not stop bleeding.
This makes the healing of this small cut impossible. Far more importantly, however, the issue can become a medical emergency for patients with clotting or bleeding disorders. Hemophilia is the most widely known example, yet several are relatively common with millions of cases in the US.
Plasma is the clear, yellowish liquid portion of human blood and is largely made of water. The remaining 5% consists of various proteins, clotting factors and other natural chemicals, and electrolyte salts. As a percentage, about 95% of normally hydrated human blood is made up of plasma fluid.
What happens during an appointment for Platelet Rich Plasma injections?
PRP therapy is performed by a physician, normally an orthopedic specialist Medical Doctor (MD) or Doctor of Osteopathy (DO). If the area is below the knee PRP is usually performed by a Doctor of Podiatric Medicine (DPM).
Physicians at Center for Joint Health injecting PRP into the kneeJust as all injuries are slightly different so are all PRP treatments. Your doctor will first take a complete medical history and perform a physical exam of the injured area. If the injury is small and it’s obvious which ligaments or tendons are involved then treatment is simple. An example is a badly sprained finger. To a trained physician it’s obvious which structures are damaged and they can be injected quite easily.
How is Platelet Rich Plasma (PRP) solution made?
Before any injections can be made into an injured knee or ankle the PRP solution itself must be produced. This fluid is derived from a patient’s own blood, making it an autologous blood product (“auto” means “self”).
By its very nature, PRP is free of all prescription and non-prescription drugs and other synthetic chemicals. Once prepared, if the solution used “as is” then the ensuing treatment is completely natural in the holistic sense.
While some physicians choose to add compound which increase the effectiveness of PRP solution this isn’t necessary. Yet even when present these additives are typically all natural themselves. If not, they’re almost always simple, well-tolerated medications with negligible side effects.

Collection of prp:
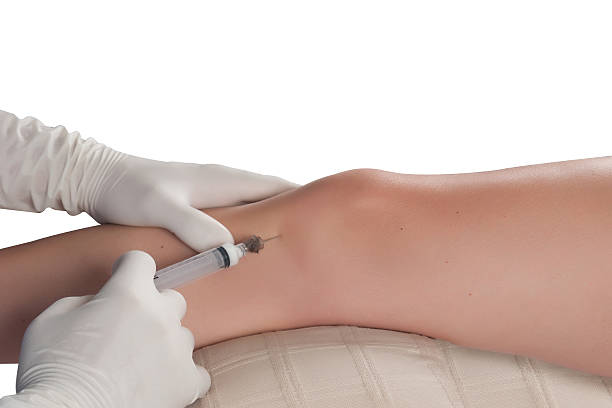
The first part of the production process is obtaining enough of a patient’s blood to produce the desired amount of PRP. Depending on how much is needed this is usually no more than 2 vials. These vials are obtained in exactly the same fashion as any other medical blood-draw. They’re most often performed by a phlebologist, or blood-draw technician. In other cases, the doctor themselves, a physician’s assistant, or registered nurse may do the physical collection.
Preparation of prp:
Once drawn, the full vials are placed in a medical centrifuge used to prepare blood products. When spun at very high speed for several minutes the blood begins to separate into 4 distinct layers:
- Red Cells—the heaviest, bottom layer. This makes up about 40-45% of the initial sample.
- White Cells—the next layer up can be seen as a very thin, whitish “buffy coat.” This layer is indeed extremely thin and makes up less than 1% of the total volume
- Platelet Rich Plasma—the straw-colored fluid immediately above the buffy coat has very high concentrations of platelets and other healing factors. This layer comprises around 5% of the total volume.
- Platelet Poor Plasma—the increasingly clear fluid above the platelet rich layer. This makes up the remainder of the vial.
What Are Some Factors That Can Affect The Outcomes of PRP Injections?
There are multiple factors that can affect the outcome of PRP injections, they can influence with recovery and healing as well, so look out for them. Here are some of them!
- Patients Health:
Age: The younger you are, the more active your platelets will be, which will surely lead to better outcomes.
Overall health: Healthy people with no chronic conditions such as diabetes, obesity, people who exercise regular and people who do not smoke and drink can get amazing results from PRP therapy, thanks to a healthy working body.
- Conditions That Need To Be Treated
PRP is known to work much more efficiently on conditions like mild arthritis, tissue injuries, and tendonitis. However, severe or serious conditions like extensive cartilage damage, or osteoarthritis may need stronger treatments and PRP may not be as effective. Furthermore, the chronic or serious your injury or condition is, the longer it will take time to heal than the less serious ones.
Can PRP Injections Be Repeated? If yes, Then How Often?
Yes, fortunately it’s possible to repeated PRP injections! Generally, patients receive 1 to 3 initial injections spaced 4-6 weeks apart. However, for chronic conditions such as osteoarthritis, injections might be needed more often every 6 to 12 months. A proper spacing between injections is important to allow the healing process and if improvement is seen the number of follow-up injections is reduced.
Can PRP Injections Prevent The Need For Surgery In Some Cases?
Yes, luckily it’s possible to prevent the need of surgeries in some cases if you are already getting a PRP treatment. These cases can be for conditions like tendon injuries, mild arthritis, or soft tissue damage. PRP promotes natural healing and reduces pain in the affected area allowing patients to manage conditions without the need of complicated surgeries.
Final Preparation of prp:
At this point your doctor will extract the Platelet Rich Plasma solution from the vial. Any desired compounds can be added, and the resulting mixture is immediately injected into damaged tissue. This jump starts the healing process, often putting an end to chronic, nagging, painful injuries.


 Platelet Rich Therapy (PRP) Treatment for Chronic Tendon Injuries.
Platelet Rich Therapy (PRP) Treatment for Chronic Tendon Injuries.