Effective Fungus Toenail Treatment Options

Before and After Toenail pics
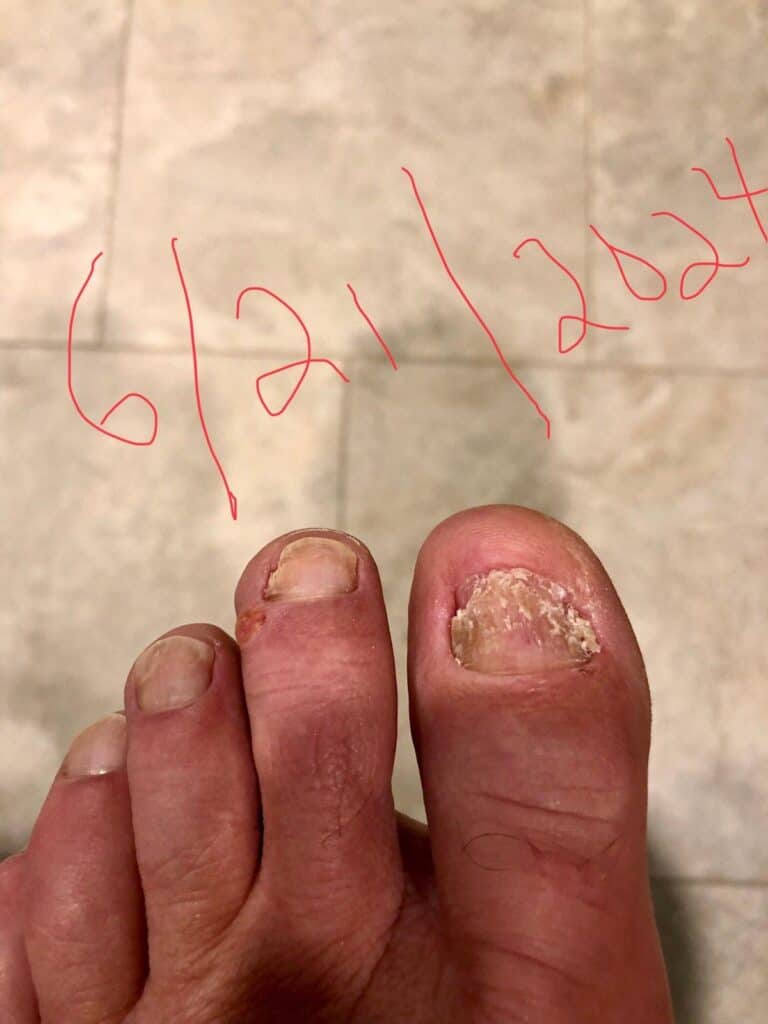
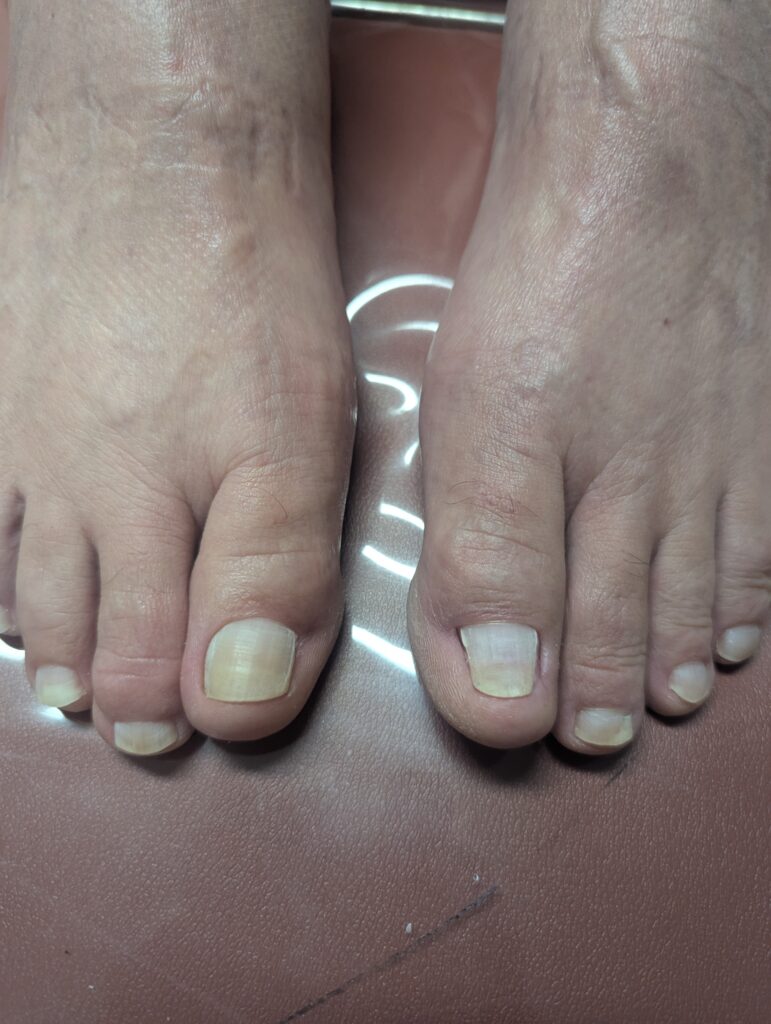
MLS-5 Laser treatment of nails 1 year after treatment.
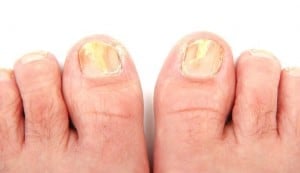
TOENAIL FUNGUS DIAGNOSIS AND TREATMENT MOON TWP
Toenail fungus – can be very embarrassing. Fortunately, there is laser treatment available for this condition. Laser treatments for toenail fungus removal were first approved by the Food and Drug Administration back in 2010. Health care professionals at Beaver Valley Foot Clinic can use several types of lasers to remove the toenail fungus. Laser treatments are popular for toenail fungus removal because they destroy and heat the harmful fungi, but they keep the healthy tissue intact.
What are Thickened Nails?
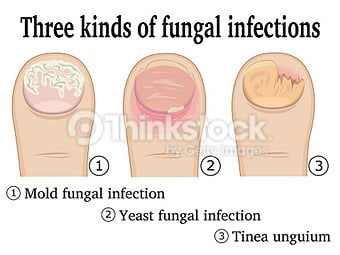
Abnormally thick or crumbling nails may be caused by injuries, pressure from shoes, fungal infections, or conditions such as diabetes, psoriasis, or vascular disease. With regular care in our office, often covered by insurance if you are at risk, can help prevent many problems from arising with these conditions.
Not all toe nail infections are caused by fungus. (Although 95% are) The rest are caused by molds, yeasts, saprophytes…
Candida (a yeast) often causes a bright red paronychia ( skin around the nail infection). there coulds even be white fluid collections of what looks like pus.
Molds are often found on people with really sweaty warm feet. Your Podiatrist can get you the correct product for your type of infection.
Ways to prevent fungal infections of the toenails.
Fungal organisms do best in warm, moist environments, making covered shoes the perfect place for them to prosper. Keep your toenails trimmed short and your feet as dry as possible, and consider the following tips:
- After bathing or showering, dry the feet thoroughly, especially the spaces between the toes. It also pays to use a hairdryer for optimal dryness.
- When in places like public pools, beaches, or locker rooms, always wear sandles. This is one of the best ways to avoid picking up a fungal infection.
- Stick to synthetic socks, not cotton. These wick sweat away instead of becoming soaked by it. Also, change your socks once during the day.
- Wear breathable shoes that fit properly.
- Wear breathable socks. Avoid tight stockings which compress the toes and can trap moisture between them.
- Don’t pick at the skin surrounding your nails.
- Use an antifungal spray or powder daily, both on your feet and in your shoes.
- If you do your own pedicures, keep your equipment disinfected–and insist that your nail salon does the same. Trust your gut when choosing a salon.
- Covering up with nail polish won’t work. It might make things look better temporarily, but will ultimately make the problem worse, as it seals in moisture, providing an even better environment for fungus to multiply.
The organisms which cause fungal infections of the toenails are very hardy, making fungal nails notoriously difficult to cure. They can enter the nail and the surrounding skin through nearly microscopic cracks, or the tiniest separation between the nail plate and the underlying nail bed.
OTC Products
Many over the counter (otc) products exist which claim to treat fungal nails effectively, and for all practical purposes they don’t work. They might be (somewhat) effective at preventing reinfection, but they generally aren’t strong enough, and more importantly can’t penetrate the nail. The only exception appears to be a prescription product called Penlac (ciclopirox), which in studies fared better than a placebo. See your podiatrist for the most effective medication geared toward your particular problem. Often the offending organism can be identified by the newer DNA testing of the nail bed material. This is available locally at Beaver valley foot clinic!
Vinegar and other do-it-yourself remedies don’t work
Dr Teimouri DPM says that over-the-counter (OTC) medications from the drugstores, whether they’re creams or the brush on type, don’t work in the vast majority of cases. Why? Because they can’t penetrate the nail, and can only be worked so far under the nail. She doesn’t recommend at home folk remedies such as vinegar soaks, tea tree oil, or bleach, either. “They don’t work. It’s that simple,” she says.
At the end of the day, treating toenail fungus is a frustrating experience for many. In most cases, even a small superficial improvement would be a major improvement.
Improvement of Toenail Fungus
Mark, shares his experience with using skin resurfacing lasers to treat stubborn toenail fungus. He received treatment on all ten toes at once, after running several marathons and damaging his nails, fubgus had taken the opportunity to invade. At the same time he purchased a Podiatrically supplied topical for followup. The Podiatrist supplied topical was “an added insurance policy,” said Mark.
Did it Work?
Did it work? In Mark’s case, yes. He reports that it took over a year for the nails to grow out completely fungus free, but the final results were all he could have hoped for. The thickened yellow appearance, primarily on the nails of the big toes, had cleared up completely. “I have a Master’s Degree, and I know that things have to be studied in order to prove their effectiveness. When people ask, I tell them that it certainly worked for me, and there’s a chance it could work for you as well.” This is obviously a single case, but a growing body of evidence is beginning to back up results like those described.This leaves prescription medications as the only standard treatments which consistently get results. They’re not perfect, and they certainly aren’t a quick fix. In the case of oral antifungal meds, the course of treatment is about 10-12 weeks, and the entire nail must then grow out for the final results to reveal themselves. This can take over a year. Concerning oral medications, however, side effects are by far the largest issue. Minor side effects are common, such as nausea, diarrhea, and skin rashes, and potentially severe and permanent liver damage occur in some patients. This type of medication has earned the reputation of being extremely hard on the liver, and without routine lab-work to monitor liver function there’s simply no safe way to take oral antifungals. What’s worse, even if all goes well, there’s a chance that the infection will return within a year.
How does toenail fungus affect the appearance and health of the affected nail?
Toenail fungus, also known as onychomycosis, can have several effects on the appearance and health of the affected nail. Here are common ways toenail fungus can impact the nails:
1. Discoloration: One of the primary signs is a change in nail color. The nail may turn yellow, brown, green, or black. In some cases, it can appear white.
2. Thickening: The infected nail often becomes thicker than usual. As the fungus progresses, the thickness may increase, causing distortion of the nail shape.
3. Brittleness: Infected nails are prone to becoming brittle and more susceptible to chipping, cracking, or crumbling. This can lead to further damage.
4. Distorted Shape: Toenail fungus can cause the nail to take on an irregular or distorted shape. This may involve curling or warping of the nail.
Can toenail fungus be effectively treated with laser therapy?
Laser therapy has been used as a treatment option for toenail fungus, and some studies suggest that it can be effective in reducing fungal nail infections. However, the success of laser therapy can vary among individuals, and it may not be a guaranteed cure for everyone.
Here are some key points about laser therapy for toenail fungus:
1. Mechanism of Action: Laser therapy for toenail fungus typically works by emitting a focused beam of light that penetrates the nail and targets the fungal infection. The laser’s energy is absorbed by the fungus, which is intended to disrupt its growth.
2. Effectiveness: While some individuals may experience improvement in the appearance of their toenails after laser therapy, complete eradication of the fungus may not be achieved in all cases. Success rates vary, and multiple treatment sessions may be required.
3. Considerations: Laser therapy is often considered for mild to moderate cases of toenail fungus.
Medical Lasers for Toenail Fungus
With all of this being said, it’s no wonder that interest in using medical grade lasers to treat nail fungus is drawing interest from doctors and patients alike. One of the key selling points is the complete lack of side effects. A series of treatments is necessary, which take only about 10 minutes apiece. While this type of treatment hasn’t been FDA approved, many clinicians aren’t waiting, and preliminary results are very promising. Yet here’s another point to consider–the treatment of fungal nail infections is considered cosmetic as opposed to medical, so insurance won’t pay for your care. The price can be considerable yet varies widely from state to state and throughout different regions, yet costs have been steadily falling as this procedure becomes more mainstream.
Regardless, it’s recommended that patients try more conservative (and less expensive) methods first, many of which are covered by insurance benefits as they’re prescribed under a podiatrist’s care. If these fail, then it’s a good time to consider laser therapy.
How is laser toenail fungus treatment accomplished?
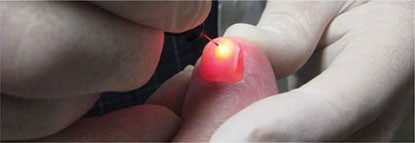
Modern skin resurfacing lasers, and all lasers for that matter, create what is known as coherent light. What this means is that the light they emit isn’t just extremely focused, it’s traveling in an actual beam. Lasers carry a tremendous amount of energy, which can instantly cause very large, short lived accumulations of heat in a target tissue. In this case the target tissue is the fungal organisms which cause toenail fungus.Laser toenail fungus removal operates by creating heat in areas of fungus.
Fungus Lasers
Lasers of several different types are commonly used to combat fungal infections. They vary in size and strength, yet even the smallest, least powerful medical grade models can produce enough heat to destroy fungus living under the nail plate.
Conditions That Might Justify Coverage of Fungus Nails for MEDICARE Patients
https://www.cms.gov/Regulations-and-Guidance/ Guidance/Transmittals/downloads/AB02096.pdf MAC Website List https://go.cms.gov/MAC-website-list Medical Review of Medicare Payments for Nail Debridement Services Program Memorandum
Systemic Conditions for nail Coverage
The presence of a systemic condition, such as metabolic, neurologic, or peripheral vascular disease, may require specialized foot care by a professional that, in the absence of such condition(s), would be considered routine (and, therefore, excluded from coverage). Accordingly, routine foot care may be covered when systemic condition(s) result in severe circulatory embarrassment or areas of diminished sensation in the patient’s legs or feet. In these instances, certain foot care procedures that are otherwise considered routine (for example, cutting or removing corns and calluses, or trimming, cutting, clipping, or debriding nails) may pose a hazard when performed by a non-professional on patients with such systemic conditions. The following metabolic, neurologic, and peripheral vascular diseases (with synonyms in parentheses) most commonly represent the underlying conditions that may justify coverage for routine foot care. Note: This list is not comprehensive.
Conditions:
● Diabetes mellitus *
● Arteriosclerosis obliterans (A.S.O., arteriosclerosis of the extremities, occlusive peripheral arteriosclerosis)
● Buerger’s disease (thromboangiitis obliterans)
● Chronic thrombophlebitis * MLN Fact Sheet Page 3 of 7 ICN 006948 September 2018 Medicare Podiatry Services
● Peripheral neuropathies involving the feet • Associated with malnutrition and vitamin deficiency * – Malnutrition (general, pellagra) – Alcoholism – Malabsorption (celiac disease, tropical sprue) – Pernicious anemia • Associated with carcinoma * • Associated with diabetes mellitus * • Associated with drugs and toxins * • Associated with multiple sclerosis * • Associated with uremia (chronic renal disease) * • Associated with traumatic injury • Associated with leprosy or neurosyphilis • Associated with hereditary disorders – Hereditary sensory radicular neuropathy – Angiokeratoma corporis diffusum (Fabry’s) – Amyloid neuropathy The following services may also be covered:
●The treatment of warts (including plantar warts) on the foot is covered to the same extent as services provided for the treatment of warts located elsewhere on the body.
In the absence of a systemic condition, treatment of mycotic nails may be covered. The treatment of mycotic nails for an ambulatory patient is covered only when the physician attending the patient’s mycotic condition documents that (1) there is clinical evidence of mycosis of the toenail, and (2) the patient has marked limitation of ambulation, pain, or secondary infection resulting from the thickening and dystrophy of the infected toenail plate.
● The treatment of mycotic nails for a non-ambulatory patient is covered only when the physician attending the patient’s mycotic condition documents that (1) there is clinical evidence of mycosis of the toenail, and (2) the patient suffers from pain or secondary infection resulting from the thickening and dystrophy of the infected toenail plate. When the patient’s condition is one of those designated above by an asterisk (*), routine procedures are covered only if the patient is under the active care of a doctor of medicine or osteopathy who documents the condition.
Medicated nail cream

Another topical option is prescription antifungal creams. When used daily for long periods of time they can prove effective, especially with the proper preparation. Before rubbing into the infected nails the patient should soak their feet in warm water. This allows the medication to penetrate deeper into the nail, hopefully reaching the fungus underneath.
Thinning the nails is also helpful, and can greatly increase the odds that antifungal creams will achieve full clearance. A simple and effective way to do this is by using a non-prescription lotion containing the ingredient urea. Another (and perhaps more effective) option is to have a podiatrist manually thin the nail with a file or similar tool.
Surgery as an option of last resort

As with almost all medical conditions surgery should be considered only after all less-invasive options have failed. In the case of toenail fungus this usually refers to topical and oral antifungals. It’s also possible that a patient may be unable to tolerate oral medications, making surgery a more attractive option.
The goal of this type of minor surgery is to allow topical antifungal medications direct contact with the fungal infection. This is accomplished by removal of the nail. The first approach is temporary removal. This is usually, although not always, successful. If the nail in question still doesn’t respond or is excessively painful then permanent removal may be necessary.
Seeking professional medical help for onychomycosis, a.k.a. toenail fungus
Onychomycosis can be extremely difficult to treat, and do-it-yourself options are largely ineffective. Also note that self-treatment can take months (or years) to be fully effective. This is why it’s almost always better to seek help from a trained podiatrist. In addition to saving time and money seeking professional help also offers the best hope for a complete cure.
When seeing a medical specialist it always pays to prepare for the appointment. Consider writing down the following information and questions to make the most of your scheduled time:
- A list of symptoms. Include all foot symptoms, even those you may think are unrelated. Also list any systemic illnesses you may have, especially diabetes and other conditions which affect blood flow to the feet.
- Your demographic information. This will include your primary care doctor’s contact information. Bring along your health insurance information as well.
- Your prescription and non-prescription medications. Be sure to include any nutritional supplements that you take on a regular basis.
- A list of questions. It’s easy to forget any questions you may have if they aren’t written down. This is the single best method of making sure that all of your concerns are addressed.
Recommended questions include the following:

- What’s the underlying cause of my condition?
- Do I need any specialized testing?
- What treatment or treatments do you recommend?
- Are there any alternatives to these treatments?
- What are the potential risks of the treatments we’ve discussed?
- Assuming that I’m prescribed medication today, are there less expensive generic options?
- Aside from my toenail fungus, are there any other conditions you’re concerned about?
- What are the estimated chances of achieving a complete cure?
- Where can I go for more information? Do you have pamphlets, brochures, or a recommended website?
How To Prevent Toenail Fungus?
Preventing toenail fungus isn’t an easy task, all you have to do just be careful and follow these tips:
- Wash Your Hands And Feet Properly
After you come back from work do not forget to wash your hands and feet properly, if you can take a bath then its even better.
Wash your hands and feet will keep you clean and all fungus and bacteria away from you.
Properly disinfect your hands before eating and avoid direct contact with an infected person.
Even if you do, don’t forget to wash your hands, these little tips will save your nail from getting infected.
- Wear Footwear Everywhere
You must wear them in places like swimming pools, locker room, gyms, parks and shower rooms because these places have high chances of having fungus and bacteria.
You should wear footwear even if you go in your yard, you don’t know what dangerous bacteria are living there, so its best to wear sandals and shoes in any public place.
- Trim Your Nails Properly
Trim them straight across, do not trim them round like your fingernails, that’s the wrong way!
If you trim your nails curve then it will be easier for bacteria to enter your body and trimming this way can cause you another problem called ingrown toenail, which is dangerous just like toenail fungus.
- Choose A Professional Nail Salon
Did you know that sometimes nail salons can be the source of nail fungus? If your nail specialist isn’t professional then this can happen.
Before choosing a new nail salon make sure they are professional and check if they wash their tools after every use or not.
If they don’t do that then they may transfer other patient’s bacteria in your nails!
If you notice these kind of actions in your nail salon then immediately change it.
Can Toenail Fungus Be Mistaken For Other Conditions?
Yes, it’s easy to mistaken toenail fungus with other conditions because of shared symptoms which can include nail, discoloration, thickening and crumbling of the nail, maybe other nail problems also show these symptoms, here are some of these:
1. Nail Psoriasis: It’s a condition an autoimmune condition that can affect both toenail and fingernails, it is recognized by putting, thickening and discoloration of nails, which resembles a lot to toenail fungus.
2. Trauma or Injury: If you develop injuries or trauma on nails then it leads to discoloration, separation or thickening of nails. But also keep in mind that an injured nail can lead to toenail fungus if it isn’t treated well.
3. Eczema or Dermatitis: Normally these are skin conditions, but can affect nails too. If they do, you might notice symptoms like brittleness and discoloration of your nail.
4. Bacterial Infections: A bacterial infection can cause greenish discoloration due to bacterial growth, similarly toenail fungus also cause fungal changes, which can be mistaken as toenail fungus.
All these conditions are as dangerous as toenail fungus and if not treated well they may lead to toenail fungus as well, so make sure you get their treatment right away!
Is Laser Treatment For Toenail Fungus An Effective Treatment?
Yes, laser treatment is extremely effective and reliable for treating toenail fungus, especially if your condition is mild or moderate! It’s because the laser emits a concentrated light that penetrates the nail to destroy the fungal infection, the deeper the infection is, the harder it will be to treat the problem, which is why it’s best to get this treatment early. Also, it’s painless and doesn’t require any serious recovery time, which means if you get this treatment early on, you can easily stop the toenail fungus and prevent future complications!
