Regenerative medicine

Regenerative medicine and sports-related injuries
 Injuries will always be a part of sports, exercise, and strength and performance training. The forces that elite athletes subject their bodies to while training and competing are almost unbelievable. Yet even light-exercise activities such as walking and cycling spawn thousands of injuries of all severity levels each year. Regenerative medicine helps you get back to top shape after injuries.
Injuries will always be a part of sports, exercise, and strength and performance training. The forces that elite athletes subject their bodies to while training and competing are almost unbelievable. Yet even light-exercise activities such as walking and cycling spawn thousands of injuries of all severity levels each year. Regenerative medicine helps you get back to top shape after injuries.
It’s also a fact that kids and sports injuries have always gone hand in hand. If anything, student athlete injuries are more prevalent (and certainly more severe) thanks to hyper-competitive high school level sports.
Right now lifestyle-level fitness programs such as Cross Fit are HIIT are also an interesting phenomenon. They’re frankly too much for most people, especially newer participants, and have become a seemingly endless source of injuries. Many (or even most) of these are due to avoidable training errors not encouraged by other, more effective approaches. HIIT is a great training system for college-level football players in peak condition who have trained intensively for years. It may be much less suitable for other athletes.
 Regenerative medicine is particularly useful because it bridges 2 specific gaps. Injuries which aren’t “bad enough” for surgery often respond well to these treatments. Situations where the injury may be causing significant problem but it isn’t worth the considerable risks of surgery. It can also be effective in cases where the particularly injury isn’t likely to respond to surgery. Chronic, repeated sprained ankles are a fantastic example.
Regenerative medicine is particularly useful because it bridges 2 specific gaps. Injuries which aren’t “bad enough” for surgery often respond well to these treatments. Situations where the injury may be causing significant problem but it isn’t worth the considerable risks of surgery. It can also be effective in cases where the particularly injury isn’t likely to respond to surgery. Chronic, repeated sprained ankles are a fantastic example.
Chronic Ankle Pain
Ultimately, it’s expected that many chronic conditions of the foot, ankle, and leg will be successfully managed without orthopedic surgery. This includes some of the most frustrating, treatment-resistant, and common conditions such as knee osteoarthritis and plantar fasciitis.
When discussing regenerative treatments such as stem cell and PRP injections the following comments are illuminating. Note that these statements were not made specifically in the context of regenerative medicine. They do reflect the sentiments of the vast majority of ethical orthopedic surgeons practicing today, however.
“Remember,” says NYC orthopedic surgeon Dr. Michael M, “there is no problem that surgery cannot make worse.” An accomplished clinician and professor at the New York University Hospital for Joint Diseases, Dr. M freely acknowledges the limitations of surgery. “It’s not perfect, and I make sure that all of my students and patients know this. Especially the students. What you really want is a great surgeon who will only operate when it’s one-hundred-percent necessary.”
Ankle Sprains Regenerative Medicine
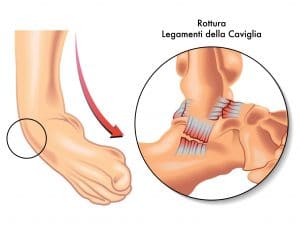
Ankle sprains are, by number, probably the most common sports-related injury that podiatrists encounter on a daily basis. During an average “textbook” sprain a person steps off of a curb or stumbles while running. The tops of the toes, or even the top of the forefoot, contact the ground first. In a fraction of a second the foot is violently forced into an unnaturally extended position. If the ankle joint is wrenched beyond its normal, healthy range of motion then significant ligament damage can occur. This is known as an inversion (rolling-inward) sprain.
Most of us know exactly what an ankle sprain feels like because it’s happened to us, once or twice. In a relatively large number of patients however, especially younger athletes, repeated sprains occur. Unfortunately, the ankle will frequently become more easily injured with each incidence. This has left many talented student athletes with “problem ankles” that persist into adulthood.
 During repeated inversion sprains, the ligaments on the front and outside (anterolateral) part of the joint become increasingly damaged. This trauma is cumulative, and the physical structure of these ligaments changes. Internally, many of the collagen fibers which give the ligament strength and flexibility are broken. The ligaments become simultaneously stretched and stiffened, and they can’t perform their main function of providing stability properly.
During repeated inversion sprains, the ligaments on the front and outside (anterolateral) part of the joint become increasingly damaged. This trauma is cumulative, and the physical structure of these ligaments changes. Internally, many of the collagen fibers which give the ligament strength and flexibility are broken. The ligaments become simultaneously stretched and stiffened, and they can’t perform their main function of providing stability properly.
PRP in Regenerative Medicine
What are platelets? What is plasma?
What most of us identify as “blood” is known by healthcare workers as “whole blood.” This incredibly complex fluid is like a living tissue in many ways. It’s a mixture of water, red and white blood cells, cell-like particles, proteins, and a plethora of naturally-occurring chemicals. Both platelets and plasma are components of whole blood.

Platelets aren’t cells, and indeed are smaller than even the smallest white blood cells. These particles perform a key role in clotting and healing. A scab which forms over a healing cut is composed mainly of platelets, cemented together by coagulated proteins.
Note that the surface of each platelet is also coated in various “chemical messengers” involved with the healing process. These healing and growth factors, mostly proteins, are thought to activate and sustain the healing response.
Plasma is the liquid portion of a person’s blood, and contains about 95% water. The remaining 5% consists of dissolved proteins (mainly albumin), fatty compounds like lipids, and salts (electrolytes). Trace amounts of clotting factors, hormones, and dissolved gasses can also be found. The unique composition of plasma allows it to support blood cells, platelets, and ultimately the entire body.
Our aim is to deliver effective, non-surgical treatments for a very wide variety of musculoskeletal conditions. This sounds like a bland, general statement, but in reality it’s extremely exciting. That’s because our treatments can improve or completely resolve the following stubborn, treatment-resistant conditions:
 Plantar Fasciitis (chronic, often severe heel pain).
Plantar Fasciitis (chronic, often severe heel pain).- Chronically sprained ankles.
- Other unstable joints.
- Advanced arthritis (including bone-on-bone). (non-foot/ankle)
- Some cases of chronic low back pain (those that don’t involve disc damage). (non-foot/ankle)
- Rotator Cuff and other shoulder injuries. (non-foot/ankle)
Many chronic joint and muscle problems like those listed above (and many others) don’t actually require surgery. This is because poor-quality or incomplete healing is the root of the issue. The treatments offered by our physicians address this underlying cause.
In many cases this involves the use of advanced imaging techniques to guide our treatments. This removes guesswork, allowing the correct placement of our premium Stem Cells and Platelet Rich Plasma (PRP) injections. Without this added precision the treatment can be less effective, or even wasted entirely.
Medicine is changing, and the medical community is becoming increasingly open to new ideas. The standpoint of Orthopedic Surgeons can be paraphrased as “there’s no problem that surgery can’t fix.” Yet today a growing number of these diehard traditionalists have realized that surgery isn’t always best for their patients. In many ways these influential doctors are acknowledging the limitations of their profession.
We offer cutting-edge, non-surgical options for many musculoskeletal conditions. You may have a chronic condition that hasn’t responded to other treatments for many years. Or you may have been told that you need surgery, and this could indeed be true. Yet your situation is unique, and it’s always best to explore all of your options. Call us today at (878) 313-3338 for a consultation. Our approach has helped thousands, and we may have an effective, minimally-invasive technique that works for you.
Are there any sports or activities that are better suited for regenerative treatments?
Regenerative treatments can potentially benefit a wide range of sports and activities. However, certain sports and activities that involve repetitive strain, impact, or high intensity may have a greater likelihood of causing injuries. Regenerative treatments might be particularly useful for athletes engaged in:
- Contact Sports:
Sports like football, rugby, and mixed martial arts involve significant physical contact that can lead to various injuries, such as ligament tears and fractures.
- Running and Jumping Sports:
Track and field events, basketball, and volleyball often involve high-impact movements that can lead to joint and tendon injuries.
- Soccer:
Soccer players are prone to injuries like ankle sprains, knee injuries, and muscle strains due to the running and sudden direction changes.
- Gymnastics:
The intense flexibility and dynamic movements in gymnastics can lead to stress on joints and soft tissues, making regenerative treatments valuable.
- Cycling:
Cyclists can experience overuse injuries affecting areas like the knees, hips, and lower back due to prolonged periods of repetitive motion.
- Tennis and Racquet Sports:
The lateral movements and repetitive swinging motions in sports like tennis can lead to injuries affecting the shoulders, elbows, and wrists.
Can regenerative medicine therapies address common sports injuries like ligament tears or muscle strains?
Yes, regenerative medicine therapies have shown potential in addressing common sports injuries such as ligament tears and muscle strains. Techniques like stem cell therapy and platelet-rich plasma (PRP) injections can aid in tissue repair and regeneration, promoting healing in damaged ligaments and muscles.
These therapies harness the body’s natural healing processes to accelerate recovery and improve the quality of healed tissues. However, the effectiveness of regenerative treatments can vary based on the severity of the injury and individual response. Consulting with a medical professional experienced in regenerative medicine can provide personalized guidance on treatment options.
Typical treatments for osteoarthritis and other common ankle and knee conditions:
 Targets only symptoms. Anti-inflammatory drugs such as ibuprofen are usually chosen since they’re inexpensive and relatively safe.
Targets only symptoms. Anti-inflammatory drugs such as ibuprofen are usually chosen since they’re inexpensive and relatively safe. - These may or may not be combined with a physical therapy program.
- The next step for most patients are steroid injections
- The final (and most invasive) step being surgery. There’s no guarantee that this will work—and it may even cause unintended additional damage.
Treatments such as PRP Therapy can now be used to trigger the growth of healthy tissue. This is highly desirable, since most chronic ankle and knee conditions involve some level of tissue degeneration or arthritic process. Steroid injections and surgery simply can’t accomplish this. Most patients will see some level of improvement, even for treatment-resistant conditions, up to and including complete recovery. The downtime associated with these minimally-invasive procedures is much less than that of traditional knee surgery.


 Targets only symptoms. Anti-inflammatory drugs such as ibuprofen are usually chosen since they’re inexpensive and relatively safe.
Targets only symptoms. Anti-inflammatory drugs such as ibuprofen are usually chosen since they’re inexpensive and relatively safe.