Eczema Treatments Eczema Causes

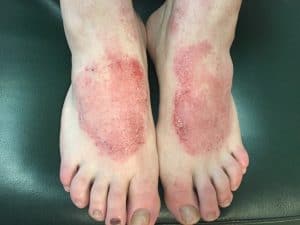
symptoms of eczema
The symptoms of eczema are typically not severe. Atopic dermatitis’ most typical signs and symptoms include:
- scaly, dry skin
- a skin blush
- itching
- weeping, crusty, or open wounds
- To get rid of their symptoms, those with
- severe eczema may require more rigorous treatment.
- Infections of the skin can also result from persistent rubbing and scratching.
Widespread Eczema
Eczema can also become pervasive and severe. In very serious cases, it can cover a large percentage of the skin’s surface. Each case is unique and therefore different. Several variables can influence the severity of your case. These factors include:
- the sensitivity of your skin,
- the length of exposure to the irritant(s) and
- the class and efficacy of the treatment(s).
If your eczema shows signs of scabing, oozing, cracking and/or bleeding it is time to seek medical attention. The worse the condition, the more likely it becomes that an infection will take hold. As eczema spreads, the chances that the skin will break or crack increases.
Eczema Treatment and Outcomes
Dermatologists and clinics that specialize in skin care are uniquely qualified to treat psoriasis and eczema. Since these two skin conditions result from different causes, it should come as no surprise that treating them uses different techniques. There may be some similarities in treating the symptoms, but the overall objective of treatment and therefore therapeutic modalities used, will be distinct.
Eczema on Legs Treatment
Similarly to psoriasis, medical professionals will likely first recommend a topical corticosteroid cream to treat eczema. There may also be over-the-counter creams that can help treat the itching. Additionally, there are some effective treatments that involve using a cream as a barrier to protect the skin from irritants and infections. This can give the skin time to heal.
Topical creams can be used in conjunction with wet bandages. This technique requires medical supervision. In some severe cases, it is performed in the hospital under constant monitoring.
More serious cases of eczema may require stronger antibiotic creams or systemic prescription medications such as oral corticosteroids (prednisone). There are potential serious side effects so they can not be used long term.
Counseling can also be used to help people avoid scratching the affected areas. People also find that talking about their condition with others who have it, can help them from feeling isolated and embarrassed.
Diagnosis of Eczema on the Legs and Feet
Eczema likes to grow in the folds of the body. On the legs, this means in the creases at the back of the knee or the front of the ankle. Sweat and other irritants from clothing and the air can get trapped in these folds, causing prolonged exposure. On top of this, the skin at the joints rub together frequently, further causing irritation. This creates the perfect environment for atopic dermatitis to take hold.
If not quickly treated effectively, eczema on the backs of the knees can become very difficult to remedy. Because of its location, it tends to be very irritating and painful. It is not uncommon that irritation and friction from clothing will cause significant discharges of blood and pus. These cases also have a high risk of infection.
Psoriasis and Dry Skin
Although many cases of psoriasis present with patches of dry or scaly skin, this is not always the case. Sometimes the large red patches show no signs of scales. With time, the red patches of psoriasis can build up a layer of dead skin cells, producing visible scales and peeling.
If you do have scales on your skin, do not pick or pull at them. They should be allowed to fall off on their own. If removed with force, the skin may break, bleed and become infected. You can however, use the palm of your hand to gently brush the area, removing small pieces of loose skin.
In some cases, the patches may develop a very thick layer of white, dead cells before beginning to shed scales.
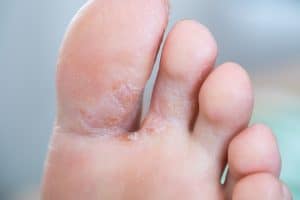
Eczema On Hands and Feet and Dry Skin
Patches of dry skin is one of the hallmarks of eczema. The skin can become extremely dry. As the skin dries, it becomes fragile making it prone to cracking. As the skin starts to peel, it may look like a peeling callus, blister, or a sunburn. The cracks and peeling skin need to be treated carefully to avoid infection.
Removing the skin may or may not expose raw skin or open wounds. They need to be handled with care to minimize the risk of introducing a bacterial or viral infection.
Eczema Symptoms
- Your skin will become itchy (almost always) before a rash appears from eczema.
- You may notice patches of dry, itchy skin on any part of your body, but usually on the hands, face and neck, or legs. Skin may feel thicker.
- Severely dry patches of skin may develop open sores with crusts and become infected if scratched.
Eczema Causes
The exact cause of eczema is not known. The most common type of eczema, which is atopic dermatitis, resembles an allergy, but the skin irritation is not an allergic reaction. It is seen in children more often than in adults. The current consensus is that the cause is a combination of factors, including:
- Genetic factors
- Immune system abnormalities
- Harsh environments
- Activities that cause skin to become sensitive
- Defects in the skin barrier that allow moisture out and germs in
What We Do Know About the Causes of Eczema
Eczema is not contagious. You can’t catch eczema by coming in contact with someone who has it.
Eczema often occurs in families. This implies a genetic role in the cause. A major risk factor is having relatives who had or have:
- Eczema
- Asthma
- Seasonal allergies (hay fever, pollen allergies, etc)
Mother’s age at time of birth has effect. It has been observed that children born to older women are more likely to develop eczema than children born to younger women, although it is not clear why.
Environment has a role. Children are more likely to develop eczema if:
- They are in a higher social class
- Live in colder climates
- Live in urban areas with higher levels of pollution
Eczema is not an allergic reaction. Even so, a large number of children who have eczema also have food allergies. In fact, doctors also know that a large percentage of children with severe eczema will develop asthma or other allergies later. But this does not mean that certain foods that are common food allergens (such as dairy, eggs, and nuts) cause eczema or make it worse. Before removing any foods from your child’s diet, consult your child’s doctor to be sure nutritional needs will be met.
What Triggers Eczema?
There are things that, although they do not cause eczema, will make an irritation or rash occur or become worse. Certain fibers such as wool and some man-made fibers are prime examples.
Symptoms of Eczema:
There are many different types of eczema, and they cause different symptoms, which include:
- Redness. The affected skin may be blotchy or red, and may even bleed.
- Itching . Itching can often be so intense that it will sometimes cause a person to damage their skin by scratching it.
- Scaling. Due to surface skin can flaking off, skin can appear rough and scaly.
- Blisters. Blisters may form and become crusty or ooze fluid.
- Cracking. Extreme cases can cause the skin to develop fissures, which are painful deep cracks.
Eczema can flare up and cause sudden, severe symptoms, or can be a chronic problem with less severe symptoms.
Types of Eczema:
Eczema Treatments Eczema Causes
Atopic dermatitis, the most common form of eczema, affects people who also have:
- Pollen allergies such as hay fever
- Asthma
- Family history of eczema, asthma, or hay fever
- Defects in the skin’s barrier, allowing moisture out and germs in
This type usually begins during childhood or even infancy, but can occur at any age.
Most often, it affects skin on the:
- Face
- Hands and feet
- Inner elbows
- Back of the knees
Over time, scratching the skin can cause it to become thicker and inflamed. Scratching can also cause infections in the raw area.
Irritants that can make symptoms of atopic dermatitis worse include:
- Soap
- Rough clothing or irritating fabric
- Household chemicals
Other allergy triggers such as certain foods and dust mites can also make symptoms worse.
How Does Skin Hydration Affect The Severity Of Eczema?
Skin hydration plays a significant role in managing severity of eczema, as eczema compromises skin’s natural barrier which makes it more susceptible to dryness, irritation and infection. Here’s how proper hydration helps you out:
- Restoring Skin’s Barrier: If you moisturize your skin daily then it will restore skin’s protective barrier which reduces water loss!
- Reduces Flare-ups: Hydrated skin is much less likely to crack because of the moisture, on the other hand dry skin has high chances to crack which leafs to inflammation, and flare-ups.
- Soothing Itching And Irritation: With no dryness on your skin, you won’t feel itchy at all, and the discomfort associated with it will be gone as well, which improved ves overall skin comfort.
Is Moisturizing Skin Alone Enough To Manage Eczema Symptoms?
Yes, moisturizing alone can easily help you manage eczema symptoms especially in mild cases as it will help you restore skin’s barrier which reduces dryness and irritation. However, if your case is moderate or severe then it might not be enough, you night need additional treatments like topical steroids or prescription based medications to control inflammations and flare-ups.
How To Prevent Eczema From Returning After The Treatment?
Here are some strategies to help you prevent eczema from returning:
- Moisturize Regularly: As mentioned earlier, daily moisturizing can help restore skin’s protective barrier and help with inflammation and flare-ups. Feel free to try some fragrance free moisturizers for good results.
- Avoid Known Triggers: identify and try your best to avoid allergens or irritants such as fabrics, soaps, or detergents to avoid flare-ups.
- Take short and lukewarm showers: Hot water will strip away skin’s natural oils which worsens eczema, therefore pat your skin dry and moisturize immediately after bathing.
- Manage Stress: Stress triggers eczema flare-ups, so practice stress managing techniques such as meditation and regular exercises.
Eczema Treatments Eczema Causes
Treatments of eczema include: (best cream for dermatitis on feet)
- Eczema cream products to moisturize the skin
- Steroid creams
- Drugs that control the immune system including dupilumab (Dupixent), which is given as an injection every two weeks, and crisaborole (Eucrisa), a non-steroid ointment that is applied twice a day
- Antibiotics (if infection is present)
- Ultraviolet light, sometimes with a drug called psoralen
- See your Podiatrist
How to avoid eczema in winter? Tips and suggestions
Eczema can be the most irritating skin issue one can have particularly in winter. Many people think that eczema is genetic and you get it since your childhood, they do not pay much attention when they come across the regular symptoms of eczema which are not quite severe.
Eczema is of different types, it is not always flaky rough skin, but a red, irritating and burning skin condition can also be termed as eczema. A person who is atopic is more likely to get eczema, as their skin will be allergic to different kinds of allergens. Not many people know this, but asthma is also a kind of eczema.
You will be surprised to know that almost 3 percent adults, and 10 to 20 percent infants are suffering with eczema, and are allergic to different skin allergies. Unfortunately, there is no cure for eczema, and you will have to confront the complications on and off for life. Choosing the best clinic, and physician to help you fight off the eczema is extremely important, otherwise, the condition might become worse, making it a nightmare.
The triggers of eczema
To treat eczema, especially when it is the allergen season, you need to learn the triggers also. Most people suffer eczema because they do not know what triggers the allergy. You might not need to go through different tests to understand the allergen, but in some cases, tests are necessary to diagnose.
The following are some common triggers of eczema.
- Food allergies
- Cold air.
- Hot weather.
- Water
- Stress
- Fabrics
- Scents
- Detergents
- Air borne allergens.
- Exercise
- Hormonal change
- Skin infection
How to avoid and control eczema attacks
Avoid those foods : eczema allergy food list
Sugars, and excess carbohydrate can cause eczema. You should maintain a controlled diet when fighting eczema.
Chronic Skin Problems
Although they are not curable, chronic skin problems can be effectively remedied with lifestyle changes and/ or drug treatment.
- •Eczema
- This is the term used for the group of conditions that make the skin irritated and/or inflamed.
Natural Remedies for Eczema – what relieves eczema
Eczema can often be remedied by some simple lifestyle changes, such as changing the products you use in your home and the clothes you wear.
- Avoid long hot showers and baths, and instead use lukewarm water for no longer than 10-15 minutes. Use mild, natural soap, or body cleanser. Avoid harsh additives and chemicals. Gently pat skin dry, and apply moisturizing lotion over your entire body.
- Avoid wool or mohair or any fabric that irritates your skin.
- Avoid tight-fitting or scratchy clothing.
- Avoid scratching if you have a rash. If you cannot control this while sleeping, wear gloves to bed.
- Sweating can aggravate the rash, so avoid strenuous activity during a flare-up.
If the above precautions do not seem to help, then the following should be tried for alleviating the rash.
- Using hypoallergenic soap, cleanse the affected area daily. Afterward, apply use lubricating lotion or cream.
- Diphenhydramine (Benadryl) in pill form may be taken to relieve itching. Do not use during the daytime however, if you need to drive a car or operate machinery, as it will make you drowsy. Another option that may not make you sleepy is loratadine (Claritin) or xyzal (levocetirizine).
Try to avoid stress during this time, both mental and physical. Eat right, exercise lightly, and get plenty of sleep to help you stay healthy and lessen the chance of flare-ups. Eczema rashes are easier to control than to cure.
Can lifestyle changes help improve eczema symptoms?
Yes, making certain lifestyle changes can help improve eczema symptoms and manage flare-ups. Here are some lifestyle adjustments that may have a positive impact:
- Moisturize Regularly:
Apply moisturizers daily to keep your skin hydrated and create a barrier that helps prevent moisture loss and irritation.
- Choose Gentle Cleansers:
Use mild, fragrance-free cleansers and avoid harsh soaps that can strip your skin of natural oils.
- Bathe Wisely:
Take short, lukewarm showers or baths and avoid hot water, which can dry out your skin.
- Avoid Scratching:
Keep your nails short and wear soft gloves at night if scratching is a concern to prevent skin damage.
- Wear Comfortable Clothing:
Choose breathable, cotton clothing and avoid scratchy fabrics that can irritate your skin.
- Identify Triggers:
Keep track of factors that seem to trigger your eczema flare-ups, such as certain foods, stress, or environmental allergens.
- Manage Stress:
Practice stress-reduction techniques like deep breathing, meditation, or yoga, as stress can exacerbate eczema symptoms.
Is eczema related to allergies?
Yes, eczema can be related to allergies, although the relationship is complex. Eczema, also known as atopic dermatitis, is considered an allergic condition and is often part of a group of conditions known as the “atopic triad,” which includes eczema, allergic rhinitis (hay fever), and asthma. These conditions often coexist and can share similar underlying causes.
Eczema itself is not an allergic reaction, but it’s commonly associated with allergic reactions and sensitivities. Many individuals with eczema also have allergies to environmental triggers such as pollen, dust mites, pet dander, and certain foods. Exposure to these allergens can sometimes worsen eczema symptoms or trigger flare-ups.
Additionally, individuals with eczema often have a compromised skin barrier, making their skin more susceptible to allergens and irritants. This can lead to a cycle where allergens penetrate the skin, leading to inflammation and worsening eczema symptoms.
Call Your Doctor If…
- During a flare-up, you are exposed to anyone with a viral skin disease such oral or genital herpes, as evidenced by the appearance of lesions or cold sores. Having eczema puts you at increased risk of contracting the herpes simplex virus.
- You develop numerous blisters in the affected area that are painful, small, and fluid-filled. This could be eczema herpeticum, which is a rare but potentially serious complication. (It is caused by the herpes simplex virus.)
- You develop yellowish to light brown crusty or pus-filled blisters over existing patches of eczema. This may indicate a bacterial infection that should be treated with an antibiotic.
- You have a family history of eczema or asthma and develop an itchy rash.
- The rash doesn’t improve within a week of treatment with over-the-counter hydrocortisone creams. You may need more aggressive treatment.