Blood Clot in Foot – Symptoms & Treatment

What to do if you suspect a blood clot?
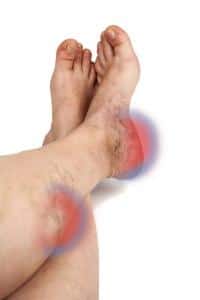 If you or someone you love suspects a blood clot, seek medical attention right away. The longer you wait, the higher your chance of developing a highly dangerous clot in one of your organs. Visit your doctor or go straight to the emergency room immediately. Clots can be life-threatening. You will want the peace of mind of a proper diagnosis. Your doctor may prescribe a blood thinner and monitor the clot. Surgery or the direct application of a clot-busting drug via a thin tube to the site of the clot may be needed. Clots are a dangerous condition that can travel through the circulatory system to anyplace in your body. If left untreated, they can become deadly. You won’t know for sure if you have one without undergoing a proper examination by a healthcare professional.
If you or someone you love suspects a blood clot, seek medical attention right away. The longer you wait, the higher your chance of developing a highly dangerous clot in one of your organs. Visit your doctor or go straight to the emergency room immediately. Clots can be life-threatening. You will want the peace of mind of a proper diagnosis. Your doctor may prescribe a blood thinner and monitor the clot. Surgery or the direct application of a clot-busting drug via a thin tube to the site of the clot may be needed. Clots are a dangerous condition that can travel through the circulatory system to anyplace in your body. If left untreated, they can become deadly. You won’t know for sure if you have one without undergoing a proper examination by a healthcare professional.
If you are experiencing any of the following symptoms, go straight to the hospital:
- Trouble breathing
- Chest pain
- Vomiting up blood
- Blood in your stool
- Dark foul-smelling stool
- Fainting spells
- Pain of numbness radiating into the left arm
- Slurred speech
- Droopy face
- Seizures
- Quick-onset confusion
What can I do to prevent a blood clot from forming?
You can take action to lower your odds of developing a blood clot. Follow a healthy diet low in fat, maintain a healthy weight, don’t smoke, and exercise regularly.
You should also:
- Avoid sitting for a long period of time, especially during a long flight or after surgery.
- If you have a desk job, set your alarm to remind you to get up and move at least every two or three hours. While sitting, flex the muscles in your legs, feet, and toes.
- Talk to your doctor about tight-fitting compression socks or garments. They may be able to help regular blood flow.
- Make an appointment with your healthcare provider. He or she may recommend taking a clot-fighting blood-thinner, sometimes called anticoagulants.
What is May-Thurner Syndrome?
May-Thurner syndrome (MTS) is a medical condition that increases one’s chances of developing blood clots. Also known as Iliac Vein Compression Syndrome, MTS occurs when the right iliac artery presses against the left iliac vein pinching the vein. This compression can cause damage to the vein and increase the risk of developing deep vein thrombosis (DVT) in the left leg. DVT is characterised by a potentially dangerous blood clot in the left leg. The clot can completely or partially block proper blood flow through the vein.
What are the warning signs for May-Thurner Syndrome?
Warning signs for MTS are subtle and very often go unnoticed. Because of this, most people do not realize they have MTS until a DVT presents itself. Individuals who experience symptoms should seek treatment. Symptoms include:
- discoloration (red or purple) of the skin,
- enlarged veins in the leg,
- leg is warm to the touch,
- swelling,
- tenderness or
- pain in the leg.
While the condition of DVT alone isn’t life-threatening, if the blood clot breaks free it has the potential to travel through the bloodstream and become lodged in the blood vessels of the lung (known as a pulmonary embolism). This is a serious and life-threatening condition.
DVT can also lead to pulmonary condition in the legs called post-thrombotic syndrome (also known as chronic venous insufficiency link). Post-thrombotic syndrome is characterized by:
- a pooling of blood in the leg,
- chronic leg swelling,
- increased pigmentation or discoloration of the skin,
- increased pressure and
- leg ulcers (known as venous stasis ulcers.)
I’ve never heard of May-Thurner Syndrome. What is it?
May-Thurner syndrome is rare. It is a vascular disorder that affects a vein in your pelvis. The right iliac artery presses against the left iliac vein, causing it to restrict blood flow. This is the vein that returns blood from your pelvis and legs back to your heart. The added pressure of the vessels pressing against each other will can cause one or both of them to narrow, impeding the blood from flowing properly. It may also cause scarring leading to a thickening of the wall. The constricted flow of blood in the leg can cause a variety of other symptoms and conditions in your legs or feet. The most problematic is perhaps a blood clot. Many people with from May-Thurner syndrome will go years without symptoms or a proper diagnosis. Over time May-Thurner syndrome can lead to:
- Swelling in the leg.
- Chronic venous insufficiency (CVI). CVI is a condition where the blood will pool within your veins, causing pressure, swelling, skin changes and venous ulcers or sores that will not heal on their own.
- Deep vein thrombosis (DVT). DVT is a blood clot in that occurs in a vein located deep below your skin. If a DVT breaks loose a moves to your lung, heart or brain it can lead to life-threatening emergencies. For example: a heart attack, stroke or a pulmonary embolism (a blood clot in your lung)
How will I know if I have May-Thurner syndrome?
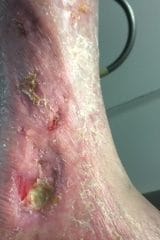
- Swelling, heaviness, or a feeling of fullness in your leg or foot.
- Sores or venous ulcers on your legs or feet that don’t heal by themselves.
- Newly appearing varicose veins in your legs.
In many cases, patients have no symptoms and can go undiagnosed for years. Only when a deep vein thrombosis (DVT) develops, do many become aware of their condition.
Some symptoms of deep vein thrombosis (DVT) are:
- Swelling in the leg(s).
- Pain and/or tenderness in the leg(s).
- Changes in skin color (such as redness).
- Skin that is warm to the touch.
How To Tell If Blood Clot Us Forming In Leg?
If a blood clot or a deep vein thrombosis is forming in your leg then it will come with some noticeable symptoms, which can include:
• Swellings in the affected leg
• Pain, tenderness and discomfort especially when standing or walking
• Feeling warmth when touching legs
• Discolored areas on legs
• Heavy or achy sensations in legs
• Veins near the skin becoming more visible than usual
These can some early symptoms, if you notice them the seek medical treatment right away, as ignoring blood clots or DVT for too long can lead to serious complications.
What The Treatment For Blood Clot In Leg Like?
When you seek medical treatment for blood clots, it will focus on you helping prevent the clot from growing further and causing future complications like Pulmonary Embolism. To do so, your will be provided with anticoagulant medications which are also known as blood thinners, most common blood thinners are:
• Heparin
• Warfarin
But if the cases are severe then your doctor might recommend thrombolytic therapy to dissolve the clots. There are also surgical options, like thrombectomy which are effective but rare as they are mostly used for large clots. Other treatments can include compression stockings to improve blood flow and reduce swelling, and lifestyle changes like regular movement, hydration and recovery prevention.
When Someone Should Seek Immediate Medical Attention For Suspected Blood Clots?
If you experience sudden or severe leg pain, swellings, redness, especially in one leg then you should seek immediate care. Some serious signs to look out for are:
• Difficulties in breathing
• Chest pain
• Rapid heart rate
• Coughing up blood
• Feeling lightheaded Or faint
These are some serious and concerning signs, they might be indicating Pulmonary embolism. Seeking medical treatment is important or it can even lead to life threatening conditions.
What are the common treatments for May-Thurner Syndrome?
You don’t have to live with the worries or symptoms of May-Thurner syndrome. It is treatable. After considering your symptoms and risk factors your healthcare provider will design a tailor-made treatment program. Any successful treatment program will effectively treat your condition while considering your lifestyle and overall health.
Common treatments for May-Thurner syndrome may include:
- Taking blood thinners or anticoagulants. These medications can help prevent blood clots.
- Thrombolysis is an intravenous procedure that we use on larger clots. In it, a catheter is feed to the site of the clot, delivering high potency anti-clotting drugs directly to the blockage. We also refer to this as “clot busting.”
- A stent is a small tube made of metal mesh that is used to hold your vein open and restore proper blood flow.
- Compression stockings are tight-fitting stocking that can ease swelling in your leg. These snug stockings are worn over your legs from your toes to knee. They apply constant pressure to your lower legs. Putting continual pressure on the area, will improve swelling and increase blood flow.
Your doctor may suggest surgery in some cases. In certain cases, surgery can be beneficial in relieving the symptoms or reducing the risks of complicating conditions brought on my blood clots. Different surgerys can be used to:
- Circumvent the section of the vein where the clot or other circumstance that is causing reduced blood flow. In this procedure, a vein is taken from another place in the body and used as a bypass, opening up the flow of blood.
- Relocate the right iliac artery. Repositioning the artery so that it is no longer pressing on the left iliac vein can open up the blood flow.
- A stent may be placed in the vein to hold it open.
What are venous ulcers?
Venous ulcers are painful sores that occur on the lower leg or around the ankle. Sometimes called venous stasis ulcers or non healing wounds, venous ulcers are lingering open wounds that don’t heal easily on their own. They frequently take, weeks, months or even longer to heal.
What are the risk factors of venous ulcers?
Various medical conditions can lead to the persistent venous ulcers. Painful venous ulcers can present themselves if you suffer from:
- Obesity
- Certain groups of medicine
- Venous insufficiency
- Diabetes
- Infections
- Venous hypertension
- Inflammatory diseases
- Kidneys failure
- Poor circulation and/or blood clots
- Varicose veins
How did I know if I have venous ulcers?
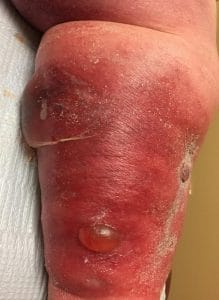
If you are at risk for venous ulcers keep an eye out for the following signs and symptoms:
- Area around the sores might be shiny. The skin may be tight and warm (or hot) to the touch.
- Discolored skin (red, purple)
- Dull ache in the leg or calf.
- Feeling of fullness or heaviness in the leg or calf.
- Swelling and cramping in the legs.
- Symptoms of blood pooling in the legs (purple, dark red, and/or brown spots. Swollen, hardened skin.)
- The edges of the ulcers are often unevenly shaped.
- Tingling and itchiness in the lower leg and/or ankle,
Stasis Ulcers: What are they?
Most commonly found on the ankle or calf, painful venous stasis ulcers are open sores that do not heal well on their own. They are typically red in color however a fibrous yellow tissue may cover them. The sores border is typically irregular. Red, purple, and brown spots may also be present on the lower legs and ankles. When suffering from venous stasis ulcers you may experience discharge and drainage. Venous stasis ulcers are common in people who have previously suffered from swollen legs and varicose veins.
Is surgery necessary to remove a blood clot in the feet?
In most cases, surgery is not the first-line treatment for removing a blood clot in the feet. The primary treatment for blood clots, including those in the feet, typically involves anticoagulant medications, also known as blood thinners. These medications help prevent the clot from growing larger and reduce the risk of new clots forming. Over time, the body’s natural mechanisms can break down the clot.
In some situations, if the blood clot is particularly large, causing severe symptoms, or if it does not respond well to medications, a healthcare provider might consider more invasive interventions.
Is it safe to massage the feet if a person has a history of blood clots?
It’s essential for individuals with a history of blood clots, especially deep vein thrombosis (DVT), to exercise caution when it comes to foot massage. While gentle massage can promote relaxation and alleviate muscle tension, it’s crucial to avoid vigorous or deep pressure massage on the affected leg or foot.
Deep tissue massage or intense pressure can potentially dislodge a clot, leading to serious complications such as pulmonary embolism (a clot traveling to the lungs). If someone has a history of blood clots, it’s advisable to consult a healthcare provider, preferably one familiar with the patient’s medical history, before considering any massage therapy. Additionally, a certified massage therapist should be informed about the individual’s medical history.
How long does it take to recover from a blood clot in the feet?
In many cases, with appropriate medical intervention (such as anticoagulant medication to prevent further clotting) and lifestyle modifications, individuals can experience improvement in their symptoms within a few weeks to a few months. Pain, swelling, and other discomfort associated with the clot often subside as the clot starts to dissolve and the affected blood vessels gradually return to normal function.
Diagnosing and Treating Venous Ulcers
While diagnosing the venous ulcers is not difficult, finding the proper cause of these painful sores can be challenging. Some Western Pennsylvania providers use a duplex ultrasound. This is a noninvasive imaging test that we use to diagnose which veins are causing the venous ulcers. The difference in this approach is that it pinpoints the abnormal vein or veins. By finding the cause of the ulceration, we can treat the venous pathology and thereby prevent the return of the ulcers once healed.
After your veins have been evaluated, your healthcare provider will recommend a personalized treatment plan based on your specific needs:
 Compression Stockings for blood clot
Compression Stockings for blood clot
- Placing the leg under constant compression is a vital aspect to healing venous ulcers.
- While, compression stockings are the most commonly used tool for this treatment, there are other methods available.
- The inward compression from the stocking will counteract the pressure from the veins of the leg and allows skin to heal.
Growth factors
- Still in the testing phase, we can apply some medications to the wound. The hope is that these medicines will promote the growth of new tissue.
Hydrocolloid dressings
- Hydrocolloid dressings is specially designed dressing that is applied over the venous ulcer.
- It promotes healing and also helps to remove any debridement (non-living tissue) from the wound.
Surgery
- Sometimes you need a minor surgery to clean the wound from non-living material. Wound debridement, as it is know, removes any non-living tissue that could keep a wound from properly healing.
Transparent dressings
- We can apply a specialized clear plastic film over the wound. The pressure from the dressing, facilitates proper blood flow.
- You should wear support stockings over the wrap to hold it securely.
Unna boots
- Similar to a cast, we can custom fit a hard boot to your lower leg. Your physician will wrap a moist gauze around your lower leg (starting at the base of the toes and going to just below the knee.)
- With time, the gauze hardens and forms a snug boot around your leg.
- The boot provides additional support for the leg, improving the blood flow in your veins, healing the ulcer more quickly.
Vein Ablation for preventing a blood clot
Vein ablation is a nonsurgical technique used to close open veins.

 Compression Stockings for blood clot
Compression Stockings for blood clot